Not all wounded patients require hospitalisation, but when they do, they must rely on complex care to prevent life-threatening complications.
Whether a patient has an acute wound, such as a surgical cut or a minor abrasion; or a chronic wound, a leg ulcer or severe burn for instance, hospital management teams require a complex plan of action.
To effectively help patients in any setting make a full recovery, science must also play its part and, in response to this demand, researchers and scientists around the globe are coming up with exciting solutions.
Chronic wounds
Chronic wounds have a reputation for their ability to cause deep-tissue damage. Their healing times are unpredictable and can often be delayed by bacteria build- up and infection.
Such wounds include venous leg ulcers, which are caused by increased blood pressure in the veins of the lower leg. This causes swelling, thickening and damage to the skin, which eventually breaks down and causes an ulcer.
Compression bandaging is the most effective method of treating venous leg ulcers, which incorporates layers to achieve a sustained level of compression over time. This treatment reduces the high blood pressures in veins and accelerates the healing process.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataThe diabetic foot also comes under the chronic wound category. Diabetic patients have high blood sugar levels and, over time, this can damage nerves or blood vessels. Nerve damage from diabetes can cause the loss of feeling in the foot and injuries can often go unnoticed, which causes ulcers and infections.
Due to delayed healing, a diabetic foot is prone to infection and, in severe cases this may lead to the amputation of a limb or the death of a patient.
Sometimes dressings alone aren’t enough to promote rapid healing and advanced technology is required.
Complex treatment
KCI Medical provides units and dressings for negative pressure wound therapy, otherwise known as Vacuum Assisted Therapy. This is a technique used in hospitals everywhere to promote the healing of wounds and burns, and fight infection, as KCI senior product manager Tina Herlihy explains, “When the unit is switched on the air is sucked out of the wound area. We call that sub-atmospheric pressure or negative pressure.”
“Due to the sub-atmospheric pressure the foam is compressed into the wound bed and the edges of the wound are softly stretched in the direction of the centre of the wound, so the total wound area is reduced. We call this phenomenon macro-strain (a clearly visible size reduction of the wound).”
The device stimulates, and therefore promotes the multiplication of cells to form fresh granulation tissue, “This total process leads to an effective wound healing,” Herlihy continues.
Ealing Hospital NHS Trust in London, England, is one health care provider which uses negative pressure to treat its patients, explains Viability and Vascular Nurse Specialist Chris Lloyd, “Topical Negative Pressure has been shown to have improved healing outcomes, particularly in chronic diabetic foot wounds which may previously have ended in amputation, but also in managing extremely large wounds which would otherwise have been almost impossible to manage effectively e.g. open abdomens and massive trauma wounds.”
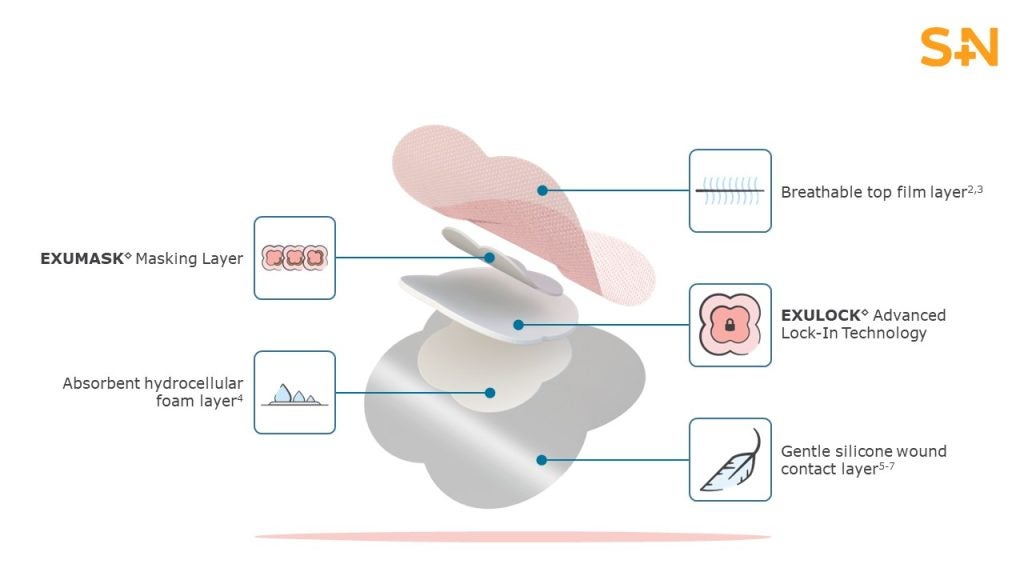
Dressings are still widely used in hospitals but the saline soaked gauze, which tend to injure surrounding granulation tissue when removed, are quickly being replaced with gauze type dressings with low adherence i.e. they don’t stick to the wound, cause pain on removal or damage new tissues, and therefore accelerate healing and reduce the chance of infection.
The Atlanticare Wound Healing Centre based in New Jersey, US also recommend advanced wound products that have increased absorption ability and contain bactericidal components like silver.
“These products have allowed the placement of dressings in the wound which last three days versus the now antiquated practice of “wet to dry” three times a day dressing change,” says the centre’s MD and Medical Director Emran Sheikh.
“These treatments allow the wound to remain undisturbed by frequent dressing changes and promote a moist wound environment for enhanced wound healing,” Sheikh adds.
Infection control
Another way to promote healing and prevent infection is to adhere to basic prevention of cross infection principles, says Deputy Head of the Department of Health Services at the University of York, UK Professor Nicky Cullum.
“Hospitals must identify the patients at risk of infection, for example those who are immunosuppressed in some way or patients with known risk factors such as ischaemia,” says Cullum. Ultimately though they best way of preventing wound infections is to prevent those wounds which are preventable and heal the others as quickly as possible.”
But often, any healing gained is often temporary, admits Cullum, “Most types of complex wounds exist because of systemic disease (venous, arterial diseases or diabetes).”
“When high quality research has examined the effectiveness of different dressings for these types of wound it tends to not find a benefit of newer expensive wound treatments over older, simpler ones. I think that this is because the underlying condition needs treating and local wound care has relatively little impact.”
The University of York is currently carrying out a five-year research programme funded by the National Institute for Health Research to carry out a study in complex wounds.
Military care
The world is entering a new generation of wound and trauma management as military and civilian surgeons and scientists team up to share expertise.
It’s true that military care is radically different to civilian care – it often involves the treatment of blast injuries and lost limbs – but surgeons’ abilities to prevent open wound infection on a muddy combat zone, mean that battlefield therapy is leading the way in the medical industry, with many healthcare authorities and hospitals picking up techniques and even opening their own trauma centres.
The Queen Elizabeth Hospital in Birmingham, UK is investing £20m to set up a National Institute of Health Research, which is set bring both military and civilian trauma surgeons together to share innovation in medical research and to benefit all trauma patients in the NHS.
Some of the techniques developed have already been picked up by the healthcare providers, including the use of tourniquets on patients with bleeding and haemorrhage injuries.
The main focus for military surgeons is to prevent complications in severe wounds and to evolve rehabilitation strategies, says Dr Pollak, chair of the Board of Specialty Societies at the American Academy of Orthopaedic Surgeons, “Far forward orthopaedic surgical care, rapid evacuation from the combat theatre and focused reconstruction at the major military treatment centres have resulted in survival and limb salvage outcomes that surpass any in the history of combat.”
ASOS hosted the 6th Extremity War Injury Symposium in January, which focused on specific challenges faced by wounded warriors and on continued efforts to join civilian and military programmes to better respond to disasters.
“All speakers were charged to focus on the big picture topics that challenged the recovery of the wounded warrior. Exciting new orthotic devices are in the development phase that could enhance the performance of the wounded warriors with injured, but not amputate, lower limbs,” adds Pollak.
Away from the battlefield, civilian hospitals are hoping to develop military precision when it comes for caring for minor and severe wounds. In the meantime, knowledge sharing about techniques and technologies must continue.