Urinary tract infections (UTIs) affect an estimated four million women in the UK every year, but in clinical settings they can often go undiagnosed or mistreated due to the inadequate state of urine sampling.
Urine from the middle of the urinary stream provides the most accurate results for medical analysis, but this is poorly communicated to patients by their physicians and even more poorly captured. Starting to urinate, stopping, positioning a tube under oneself and then starting again is both messy and undignified. However, not doing so means that the sample can be contaminated by bacteria in the urethra and on the surface of the skin, which are flushed out with the first part of the urinary stream and could corrupt the sample.
Research has revealed that as many as half of all urinary dipstick tests completed by general practitioners could be unreliable. The tests are riddled with false positives, as the sticks react to bacteria which may have been on the surface of a patient’s skin but are unrelated to the urinary tract.
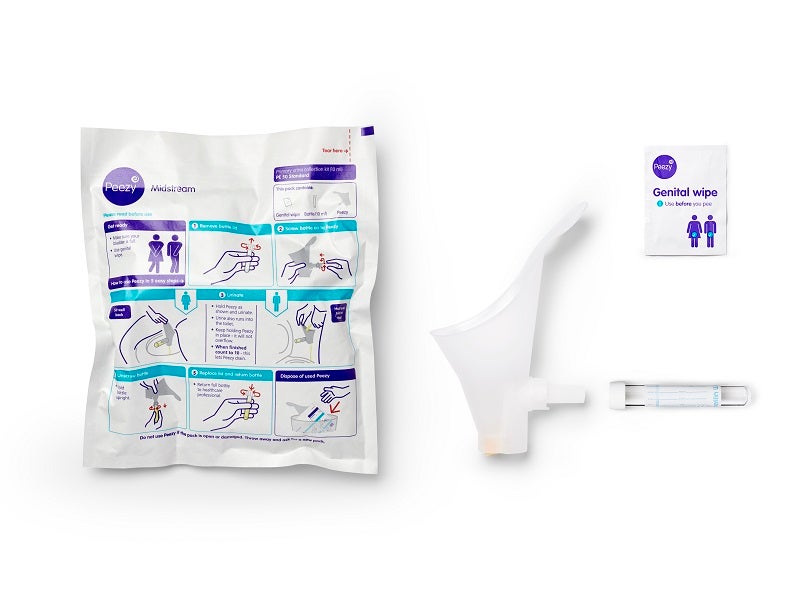
Now, London-based medtech developer Forte Medical is hoping to change all that. Peezy Midstream is a urine collection device designed to ensure that only midstream urine is collected – and it’s been making waves at the Oscars and beyond.
How does the device work?
The device’s design guarantees a midstream collection, meaning samples are more likely to yield accurate results upon testing.
“It’s a female body-shaped funnel that sits comfortably against the perineum,” says Forte Medical CEO Giovanna Forte. “You start to pee. At the end of the funnel there’s two exit points – one has got a small, compressed sponge in it. The urine collection tube screws onto the side of the funnel. The first bit of urine goes through the void with the sponge in it and the sponge expands and acts like a cork. The midstream is pushed up and into the bottle.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalData“When the bottle’s full, there’s a kind of vacuum that’s created, so that will just stay where it is and won’t get diluted with later urine; the last urine goes through the second void. The flask is designed not to overflow.”
The device has managed to reduce false positives by 70% in clinical settings. It’s a fairly impressive statistic, which becomes even more vital considering the fact that urine has a diagnostic quality on par with blood but there are very few regulations about how it is sampled and tested.
Forte suggests that both an aversion to urine as a waste product and a tendency to dismiss women’s health issues are to blame.
“Because urine is a waste product it has been slightly overlooked in terms of the quality of the sample that is being analysed,” she says. “Plus, UTIs are largely a women’s problem. Women have messy bodies, they put up with a lot of their periods, they put up with giving birth. Things don’t get diagnosed first time and we just take it as part and parcel of things.”
Four years ago, Forte Medical submitted freedom of information requests to every NHS Trust in the UK asking what their urine contamination rates were. The responses came back ranging from 1% to 70%.
Forte says: “If you had that disparity in the quality of specimen of blood there would be a national outcry. Because it’s urine people think the test can just be carried out again, without thinking of the cost or the fact that someone’s condition might get worse.”
UTIs are costing the NHS millions
Forte recently became her own case study for medical institutions’ mishandling of UTIs when she was diagnosed with an infection and given a broad spectrum antibiotic. After the drugs made no difference she returned to her doctor, who prescribed a longer and stronger course of the same antibiotic. Following this, she ended up in hospital with borderline sepsis.
Forte says: “I got to the hospital and told them that I got the same antibiotic for longer and the doctor just looked at me and said, ‘You’re joking – you’re not supposed to do that.’”
The incident highlights just how poorly UTI care can be managed. In the most recently available data, 184,000 patients had an unplanned hospital admission as a result of a UTI, costing the NHS £434m. UTIs also accounted for nearly 20% of all hospital-acquired infections.
If implemented across the NHS, it’s hoped Peezy Midstream could drastically reduce these figures.
The device has been adopted in antenatal clinics in west Hertfordshire, is in use in north Devon and is about to undergo a major trial in Birmingham. Public Health Wales started a two-part trial into Peezy’s benefits last year, and has shown cost savings and more prompt treatment for patients in general practice, leading to its introduction in surgeries across the country.
It’ll be a while before Peezy Midstream becomes the gold standard for urine sampling globally, but it’s off to a pretty strong start.
“I would urge medics and healthcare professionals to accept that this is something that needs discussion,” Forte says. “There’s no dialogue. It’s overlooked because it’s deemed to be unimportant.”