University of Utah develops robotic drill to minimise surgical time
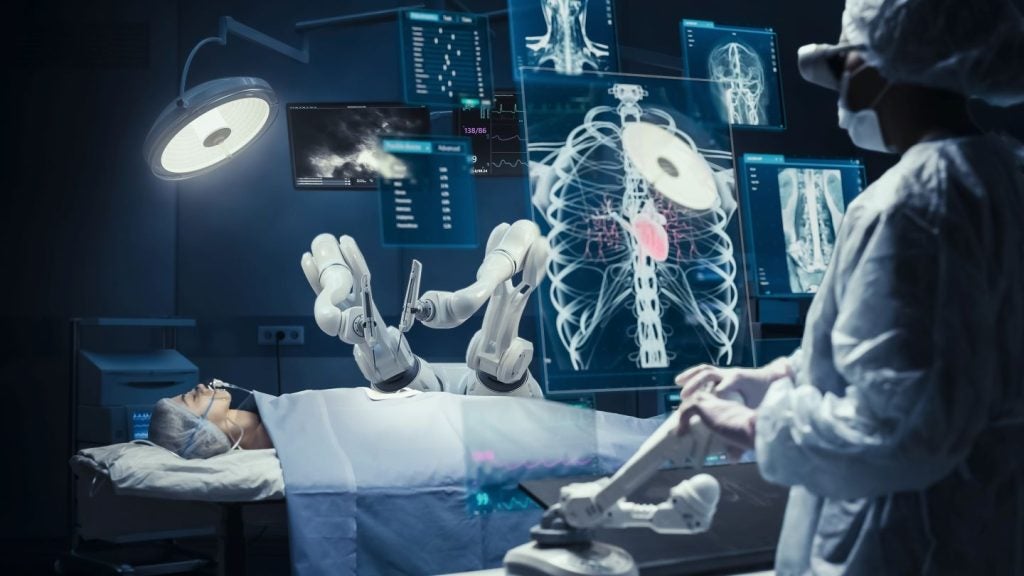
The University of Utah, US, developed an automated robotic drill with the potential to reduce complex cranial surgery time from two hours to two and a half minutes.
The computer-driven drill is able to make fast, clean and safe cuts, minimising the risk of infection, human error and surgical cost.
The device is claimed to make surgery 50 times faster than standard procedures, which require the use of hand drills to make complicated openings.
UK and China develop new low-cost graphene sensor for hepatitis diagnosis
UK and China collaborated on a new project to develop an easy, low-cost sensor for simultaneous diagnosis of hepatitis A, B and C. It uses an advanced 2D material with high electrical conductivity called graphene.
Funded by Newton Fund UK, the new diagnostic technology project is led by BIOVICI and involves UK’s National Physical Laboratory (NPL), Swansea University, China’s University of Chongqing, and CTN.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataSee Also:
Aimed to address hepatitis in China, the new project is also working towards tackling issues with the existing standard blood test methods used to diagnose the disease.
Beaumont Health develops new urine test to detect Zika virus

The US-based firm Beaumont Health developed a new urine test for rapid detection of the Zika virus.
Led by Beaumont Hospital, Royal Oak, Michigan, urology scientist Dr Laura Lamb, the research team developed a quick, simple test that is easy to administer and delivers results in 30 minutes.
The new test aims to address the concerns with current procedures, which require medical staff to draw blood and send it for a four-week analysis.
FDA authorises Cook Medical’s new device to treat esophageal atresia in infants
The US Food and Drug Administration (FDA) authorised the use of Cook Medical’s Flourish Pediatric Esophageal Atresia Anastomosis device for the treatment of esophageal atresia in infants up to one year old.
Esophageal atresia is a birth defect observed in babies and is characterised by a gap in the esophagus.
The Flourish device closes the gap by using magnets to pull the upper and lower esophagus together.
NUS develops new handheld device to treat glue ear

The National University of Singapore (NUS) developed a new handheld device called CLiKX for the treatment of patients with Otitis Media with Effusion (OME) or glue ear.
Designed to improve surgical treatment of the condition, the 185g sensor-guided device is a pistol-like applicator with a grommet tube that can be inserted into the ear with a single click.
The procedure can be performed in a consultation room under local anaesthesia, or an operating theatre under intravenous conscious sedation without general anaesthesia.
UK's ICR develops new test to predict targeted prostate cancer treatment outcome
The Institute of Cancer Research (ICR), UK, developed a blood test in partnership with Royal Marsden NHS Foundation Trust that could predict the outcome of certain targeted treatments for prostate cancer.
The test is designed to detect tumour DNA in the blood and identify the presence of numerous copies of the androgen receptor gene, which reportedly aids in cancer resistance to therapy.
Researchers evaluated blood samples from men with advanced prostate cancer in a study funded by Prostate Cancer UK, Cancer Research UK, the NIHR Biomedical Research Centre at The Royal Marsden, and ICR.
Varian introduces new human-centred system to treat cancer

US-based Varian Medical Systems introduced a new human-centred, user-friendly device called Halcyon for the treatment of cancer.
The system is designed to automate, streamline, simplify and bolster the virtual aspects of image-guided volumetric intensity-modulated radiotherapy (IMRT).
Contrary to existing older technologies that require more than 30 steps, the device involves nine stages from the start to the end of treatment and is suitable to deliver treatments for several types of cancers such as prostate, breast, head and neck.
Synaptive Medical and CSU to develop new technology to detect brain tumours
Synaptive Medical collaborated with Colorado State University’s (CSU’s) Flint Animal Cancer Centre, US, to develop a new intraoperative imaging and sensing technology for detection and treatment of brain tumours.
CSU neurology and neurosurgery associate professor Dr Rebecca Packer utilised Synaptive’s Raman spectroscopy research system to assess the clinical biomarkers with potential for use in surgical resection of tumours.
With a focus on new brain tumour therapies, Dr Packer’s research aims to create precise and less invasive neurosurgical techniques and therapies to treat the tumours.
Elekta unveils new MR/RT system with MRI scanner
Elekta unveiled its new magnetic resonance radiation therapy (MR/RT) system, Elekta Unity, at the 36th European Society for Radiotherapy and Oncology (ESTRO) meeting in Vienna, Austria, from 5-9 May.
The system comes with an integrated (1.5 Tesla) MRI scanner, advanced linear accelerator and intelligent software.
The device is designed to simultaneously deliver precisely targeted radiation doses and capture high-quality MR images to facilitate tumour visualisation and treatment adaptation.
Mel-Mont Medical develops self-collected diagnostic test for cervical cancer
Mel-Mont Medical developed a new preventive comprehensive diagnostic system for cervical cancer called Mía by XytoTest.
The new system comes with a medical device that enables self-collection of cervical cells in any setting without assistance.
The collected sample is later analysed to identify human papillomavirus (HPV) using a molecular system of real-time polymerase chain reaction (PCR).