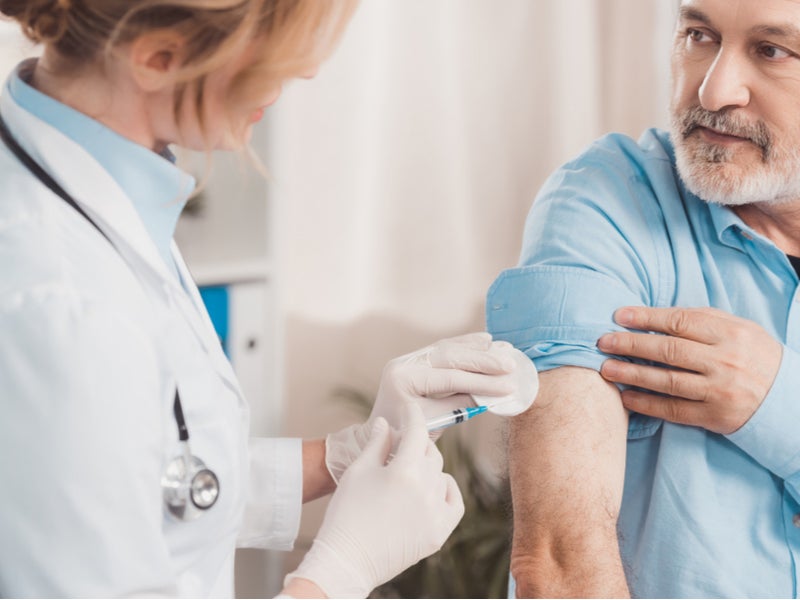
The portrait of vaccine hesitancy is often that of a misinformed parent who refuses to immunise their young child for fears the injection itself could lead to the development of more serious health conditions, such as the long-discredited link between the MMR vaccine and autism.
However, adult vaccination rates are also dropping. Across member states of the Organisation for Economic Co-operation and Development (OECD), the rate of influenza vaccination among over 65s decreased from 49% to 43% between 2005 and 2015 – a big drop, and significantly below the World Health Organization’s (WHO’s) target of 75%. It is estimated that 40,000 – 220,000 deaths per year in the European Union (EU) may be caused by cases of flu.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Several factors can be blamed for the low rates of vaccination in this demographic, including access to care and vaccine availability, but research from the International Longevity Centre UK (ILC-UK) has shown that individual attitudes towards flu vaccinations are key to shifting this behaviour.
ILC-UK found that due to patient assumptions that vaccines are limited to childhood, they lacked awareness of the importance of immunisation later in life. Many members of the public also associated flu vaccinations with being in ill health or frail, giving them a negative perception of the procedure.
ILC-UK senior research fellow Dan Holden said: “We need to reframe the messaging around seasonal flu vaccination, to make the flu jab a positive lifestyle choice just like taking vitamins or going for a walk.”
Publishing ‘Data, bots and drones’ in April 2019, ILC-UK believes that uptake rates for this and other adult vaccines can be improved through technology, which can help to counter misinformation surrounding the value of vaccination. The report presents findings from a workshop held in Brussels in 2018, where NGOs, policymakers and healthcare professionals gathered to discuss how technology could be used to support adult immunisation uptake.

US Tariffs are shifting - will you react or anticipate?
Don’t let policy changes catch you off guard. Stay proactive with real-time data and expert analysis.
By GlobalDataLeveraging social media
One issue raised time and time again was the importance of leveraging social media against the anti-vax tide.
ZN Consulting chairman Philip Weis said: “Antivaccinators are sometimes more sophisticated and coordinated than those advocating pro-science messaging.”
Social media has been used to spread disinformation about vaccines on a huge scale, risking the progress made towards eradicating yellow fever in Brazil and Polio in India. Fake stories spreading via channels such as WhatsApp have also been credited for driving vaccine hesitancy in close-knit religious communities such as New York’s ultra-Orthodox Jewish population, which has seen a huge surge in measles cases.
ILC-UK has thus urged worldwide governments and industry leaders to invest in digital health literacy for populations where it may be lacking. While the surge of anti-vax propaganda spreading across social media may seem obviously false to younger, more technologically adept individuals, older people and those who lack knowledge around the importance of vaccines are far more susceptible to it.
To bridge the generational divide, it has also been suggested that organisations reach out to Instagram influencers and YouTube stars who could encourage their young social media audience to speak to their parents and grandparents about the importance of adult vaccination.
Wearable devices
Indian medical student Richit Nagar recently devised a digital necklace that can store a person’s medical history, including their vaccination records. Designed for people living in rural parts of India where accessibility issues and lack of awareness impede vaccine uptake, the necklace is designed to be scanned by visiting healthcare workers via a smartphone, who can then give out vaccines and other care based on the records stored there.
The necklace is designed as a medallion on a black thread, a culturally important symbol of protection in many parts of India, which is intended to help integrate the device smoothly into the populations it is designed for.
Of course, different devices will need to be developed based on the different needs of populations, but internet of things technologies such as these have the potential to be more inclusive than purely text-based technology.
Artificial intelligence
Many countries lack the systems to identify at-risk adult populations who would benefit from vaccination programmes, or the tools to follow through on this information and target them for vaccination. However, the use of artificial intelligence (AI) could speed up the process of identifying people who would benefit from vaccination and reach them in a meaningful way.
Sanofi, the sponsor of ILC-UK’s report, has been working with Berg to use AI to assess different populations, races, ages and geographies to see if certain vaccines are more effective in different populations.
Another company using accessible AI to generate smarter healthcare solutions is OKRA Technologies, a start-up led by Delft University graduate Loubna Bouarfa. Its platform works on a figurative and practical level, using environmental and health data to make predictions and assessments about in-need populations, and could be used to pinpoint regions where vaccine uptake is low.
Bouarfa says: “What our system does is flag out regions that there is high population of patients in need of a certain treatment [such as a vaccine]. We then provide our pharmaceutical clients with insight, how to reach out to doctors in these regions, what messaging to use, what clinical based evidence there is about the region, so that they can help patients reach treatments.”





