In recent years, healthcare professionals have faced a succession of infectious disease outbreaks, such as swine flu, cholera and avian flu, all of which provided their own specific diagnostic challenges. Reaching a conclusive diagnosis can take some time during which the affected person may infect others. Likewise, the number of people involved may stretch screening resources to the limit, exacerbated by the difficulty of reaching specific regions or individuals.
Dealing with these factors requires a two-pronged approach. One involves ensuring the diagnostic technology is as quick and accurate as possible. The other, establishing processes to deal with the diagnostic phase as effectively as possible, and to counteract some of the problems created by specific circumstances.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Infrared fever screening
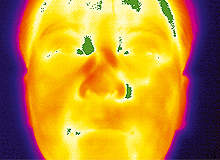
During the 2009 swine flu pandemic, there was much publicity about infrared detectors being used in airports to detect whether passengers had a fever by measuring the infrared energy they were emitting.
The major potential benefit of such equipment in hospital environments is that people can be screened quickly with minimal contact. Those with an apparent fever can then be moved out of public areas immediately and cared for by staff employing specific precautionary measures, thereby minimising the risk of further infection while more detailed diagnosis takes place.
The US Centers for Disease Control and Prevention carried out a study of such equipment in three emergency departments in New Mexico, Georgia and Illinois. Researchers concluded that the two scanners with the best results, manufactured by OptoTherm and FLIR, were reliable in identifying elevated temperature.
Portable kits
Current diagnostic tests can take up to a day because they require several manual processes, including the breakdown of a virus sample, extraction of pathogenic RNA/DNA from the sample and molecular diagnosis.

US Tariffs are shifting - will you react or anticipate?
Don’t let policy changes catch you off guard. Stay proactive with real-time data and expert analysis.
By GlobalDataThe Institute of Bioengineering and Nanotechnology has developed the Micro-Kit, a portable, all-in-one fully automated desktop system that can diagnose within two-and-a-half hours. The operator simply pipettes the sample into a self-contained cartridge, with the system automatically performing the entire sample preparation and diagnosis. The Micro-Kit has already been employed for seasonal influenza A (H1N1) typing and sub-typing, with comparable sensitivity to conventional methods.
Another intriguing development has arisen from the Bill & Melinda Gates Foundation’s projects aimed at combating killer infectious disease in the developing world. Researchers at the University of Washington have incorporated a test into a plastic card onto which a sample drop can be placed.
The card can withstand rough treatment, and does not need the controlled conditions of a medical laboratory. Clearly, a major benefit will be the ability to diagnose in the field wherever there is a need. Although the prototype focuses on malaria, the aim is also to apply the technology to other high-fever diseases including, influenza, dengue and typhoid.
Results are read off the card at the present, but the intention is to develop a system by which the clinician feeds the card into an instrument which gives a yes/no response for a panel of infectious diseases in 20 minutes or less.
Mobile laboratories
There are also a number of approaches that can impact significantly on diagnosis efficiency and effectiveness, other than the specifics of the diagnosis technology itself. When cases of avian flu were on the increase in south-east Asia, Thai authorities wanted to ensure they were fully equipped to contain such an outbreak.
Typically, it was taking laboratories three to four days to submit reports. Where hospitals were in remote areas, the process was even longer because of the time involved in transporting samples to reference laboratories.
The Regional Medical Sciences Laboratory in Khon Kaen has developed a quality, rapid-response avian/human influenza mobile laboratory for deployment in epidemic areas in the upper north-eastern region of Thailand. Not as expensive as conventional reference laboratories, it conformed fully to ISO 15189, the medical laboratories standard.
There was a big emphasis on close coordination with community leaders and health personnel to ensure activities were in tune with local needs and to enable setting up surveillance networks. Diagnosis time was reduced to six to eight hours, with inter-laboratory comparisons showing no significant divergence from results achieved in a more traditional laboratory environment.
Communication strategies
Knowledge is power, and being able to see patterns in the spread of an outbreak assists with diagnosis strategy and resource deployment. However, this is harder than it sounds, not least because there can be a significant time lag from early symptoms to concrete proof of a particular illness.
HealthMap, an internet-based infectious disease tracking system, works by drawing down information from a variety of official and informal sources. Although official surveillance sources are high quality and detailed, informal surveillance, such as media stories, social media and personal reports, can help to identify areas of concern earlier.
In relation to Haiti’s cholera outbreak, a ‘crisis mappers’ community on the ground has been sending real-time data to HealthMap via mobile phone and iPad. From the most advanced medical technology to the internet and social networking, society is using everything in its armoury to tackle the threat, and the results are transforming approaches to diagnosis.





