In many industries, the increased understanding of robotics and automation is reaping benefits and opening up efficiencies previously thought unattainable. Advances in medical robotics might not be penetrating the world’s hospitals as quickly as industrial robots are populating the world’s factories, but there is no doubt that technology is slowing transforming the way surgical procedures are being carried out.
One system that is proving particularly popular in the US (and slowly gaining ground elsewhere) is the da Vinci surgical system,developed and manufactured by California-based Intuitive Surgical.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Now on its third iteration, this system employs remotely controlled robotic arms to allow surgeons to achieve greater dexterity and vision when undertaking laparoscopic or minimally invasive procedures.
We caught up with Chris Simmonds, senior director of marketing at Intuitive Surgical, to find out how the da Vinci device measures up when it comes to the complexities of mitral valve repair and cardiac revascularisation, and whether surgeons have been able to keep up with the skills required for cutting-edge, computer-assisted surgery.
Chris Lo: What makes up the da Vinci system?
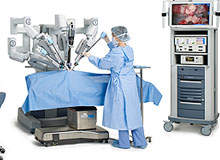
Chris Simmonds: The da Vinci system is made up of the surgeon console, which is where the surgeon sits and the patient side cart, which has the robotic arms. The third element is a vision tab, which is where all the intelligence and the computing of the system is located.
Perhaps a better way of defining it is it’s not so much robotic surgery as it is computer-assisted surgery – it’s a complete slave-master relationship, nothing happens that is not within complete control of the surgeon. What we’re doing is putting a computer between the surgeon and the patient and then allowing that computer to control these arms.
The system provides vision – you are seeing things in 3D, which you don’t see when you’re doing standard keyhole surgery through laparoscopy.
That has a huge impact in terms of seeing depth, especially when you’re doing reconstructive work like suturing.
The other thing it has is dexterity; the instruments themselves have 360 degrees of motion, so in fact the surgeon can do much finer movements than they can in an open procedure. The third element that we talk about is control; for example, we actually reduce any tremor through tremor filtration. It’s a much steadier hand, so to speak.
CL: What kinds of cardiac surgery is the Da Vinci device used for?
CS: The two procedures that make up the majority of cardiac procedures – the first one is mitral valve repair, and the second one is cardiac revascularisation. The da Vinci is used for both of those.
This is mainly in the US. We don’t have that much penetration of cardiac procedures outside the US. I think it’s to do with the adoption – the system has really been adopted faster in the US than in other countries. The cardiac procedures are more complex, so it takes a bit of time to get everybody organised.
CL: What are the benefits of using the da Vinci system in cardiac surgery?
CS: It’s two-fold. Most importantly, it offers a clinically equivalent, and in some instances a superior procedure to open surgery. The second thing is that it’s doing it in a less invasive manner, it’s the keyhole approach. You therefore get the benefit of not having a sternotomy [incision along the sternum] or a mini-thoracotomy [incision into pleural space of the chest].
Obviously, that has a huge impact for the patient, both in terms of the length of time that they stay in hospital and the recovery time afterwards. There have been a couple of papers published on mitral valve and cardiac revascularisation which both prove that Da Vinci is either clinically equivalent or superior, and there are shorter lengths of stays.
A paper done by Dr Poston in Boston, looking at coronary vascularisation, shows that you’re getting in some instances superior results. Essentially, when you do a coronary bypass, what a lot of people end up doing is taking a vein out of somebody’s leg or arm and then grafting it on to the heart. What they do with the robotic approach is they take one of the arteries that are feeding the mammaries and then re-graft that on to your heart. So what you’re doing is redirecting an existing artery that’s already in your chest, and that gives better results because it’s less likely to clog up again afterwards. The patency levels of mammary arterial grafts are much higher than those of saphenous vein grafts. The robotic approach allows you to do that.
CL: How can a system like this reduce the risk of a cardiac procedure?
CS: It’s still a cardiac procedure, so the risk is still the same. Obviously, with mitral valve, you’re still putting the body on-pump, so you’ve still got the issues related to that. In fact, on coronary revascularisation, people are doing these surgeries without having to stop the heart. That’s a different debate, about whether coronary surgery is better on-pump or off-pump. But it is still coronary surgery and the inherent risks in the operation are going to be the same because you’re putting somebody under general anaesthetic.
I think where the benefits come through is after the operation, because you take a less invasive approach. But I wouldn’t want to suggest that it’s not risky, so to speak. Any surgery is risky from that perspective.
CL: Do you think there is a general trend in surgical manufacturing pushing towards minimally invasive techniques?
CS: The simple answer is yes. This is because when a patient is faced with a choice of either having invasive surgery or a less invasive approach the patient would rather not go under anaesthetic and not have to have surgery if they can avoid it.
This less invasive approach can be surgical with the da Vinci, but equally there are other medical technologies, stents or other products – so that’s been one of the drivers of not just the da Vinci, but also of a whole plethora of other medical device products.
CL: Is there a learning curve for surgeons getting to grips with this system?
CS: What does change is the set-up. So obviously, surgeons do have to learn how to use the system itself. But using the system is pretty intuitive. Laparoscopy is counter-intuitive – for example, when you’re doing keyhole surgery, when you move your hand right outside the body, your instrument moves left on the screen you’re looking at. With the da Vinci, all that is removed, so when your hand moves right, the instrument moves right.
So there are two stages to learning how to do this. The first thing is learning how to use the system, and the second thing is what we call the clinical pathway, which is adapting those system skills to enhance your surgical skills. In cardiac surgery, that takes a lot of time. It’s not something where you can go from doing an open procedure to doing the da Vinci procedure from one day to the next. There are very specific courses that are being developed and run by some major institutions like the Cleveland Clinic and St. Joseph’s Hospital in Atlanta.
It’s a stepped process, so you’ll start off doing elements of the procedure, then gradually moving on to full procedures depending on the skill of the surgeon and the whole OR team.
CL: Does Intuitive Surgical offer other cardiac surgical equipment beyond the Da Vinci system?
CS: When you think of the system, you’ve obviously got the system itself, but you’ve also got the instruments. We do actually develop specific instruments for cardiac procedures.
‘For example, we have an atrial retractor, we have a valve hook for mitral valve repair, we have a stabiliser for revascularisation so that when you’re doing your anastomosis, especially when it’s being done on a beating heart, you can stabilise it so you can do it much tighter.
There’s a third party who we work with, who can add extra elements to the procedure.
Back in the late 90s, we very much focussed on cardiac as the area where we thought there was the greatest potential for benefit with the robotic surgical approach. To be completely honest, the first da Vinci system that we did, conceptually it was right, but from a technological perspective it wasn’t quite ready yet.
Now we’re on the third generation system, and there have been some modifications that have been done, meaning that it is now better suited for cardiac procedures. But a cardiac procedure is a very complex procedure. You don’t just have to train the surgeon, you have to train the whole OR – everybody has to be on-side, because you really do change the way the patient is treated.





