Nitinol is now accepted as a medical device material, but this wasn’t always the case. For three decades after the discovery of nitinol in the early 1960s industry struggled to find a profitable application for the material – first in the military field, and then in the electronics, consumer and automotive markets. Early efforts were hampered by three persistent problems: a lack of consistent material at a reasonable price, the inability of nitinol to perform over a broad enough range of ambient temperatures and a misunderstanding of nitinol’s complex properties.
Thirty years later, however, nitinol finally found its way into medical devices, and the exploitation of the material has since been swift and dramatic: within just a few years, nitinol went from being known by just a handful of specialists to being part of nearly every physician’s and engineer’s vocabulary.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Engineers found that it delivered an 11% spring-back strain, it could thermally recover its shape when warmed to body temperature and it applied a constant force over a long range of strains. In short, it closely matched the compliance of nature’s own materials. Two of the problems mentioned earlier could be neatly sidestepped in medical implant applications, where devices tend to be so small that high material costs can be tolerated, and the constant 37°C environment in the human body at once resolved all the ambient temperature issues. The third problem, however, continues to shadow nitinol. Many people still underestimate how different nitinol really is from conventional metals and fail to understand its properties.
FATIGUE FACTS
Perhaps the biggest misapprehension regarding nitinol relates to the subject of fatigue. Recently, several papers have been written by members of the medical community implying that many nitinol devices are not ‘fatigue safe’. A surprising number of people have concluded that nitinol is highly prone to fatigue damage.
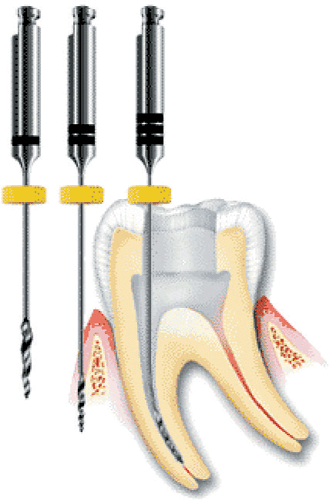
In fact, while nitinol is rather susceptible to stress or load-controlled fatigue, it is by far the most resistant metal known to high-amplitude strain-controlled fatigue environments. Several applications, such as the dental files shown in Figure 1, employ nitinol solely because of its extraordinary fatigue resistance. Most applications of nitinol in the body are best viewed as strain-controlled, so why are nitinol fatigue fractures receiving so much attention, and why are components breaking?
Nitinol is often used because of its ability to preserve the natural physiology of the body. By way of example, contrast a typical balloon expandable (BX) stent with a nitinol self-expanding (SX) stent. The former typically reduces the compliance of a healthy vessel from 6% diameter change per 100mm-Hg to less than 1% – essentially arresting the pulsatile movement of the vessel.
Meanwhile, a typical nitinol stent might retain a stented vessel compliance of 4%, continuing to expand and contract with each heartbeat. Intuitively, preserving the correct physiology seems desirable, but there is a price: the nitinol device is exposed to fatigue conditions far more severe than a conventional material – a stainless steel stent could not possibly survive in that environment, but it does not have to. Of course, one could design the nitinol device to prevent pulsatile motion as well, but then there would be no point in selecting nitinol in the first place.
MOTION DILEMMA
The debate is whether it is better to prevent native vascular movement and avoid fracture, or to allow motion and risk fracture. The answer depends upon the application. Consider the stenting of the Superficial Femoral Artery (SFA). Running from hip to knee, through muscle and joints, the SFA undergoes severe changes in geometry associated with leg movement (see Figure 2).
A nitinol stent allows an artery to continue to bend, crush, stretch and twist, while a BX stent restricts these movements (within the stented length). If stents are short, a BX stent will simply shift and concentrate the vessel movement (Figure 3) – it isn’t clear if or when that becomes problematic. If the stented lengths are long, even a stiff BX stent will be deformed, often with serious consequences, since the deformations are permanent. Thus nitinol stents are the only reasonable candidates for these dynamic environments. Like it or not, again, nitinol is chosen for the most challenging fatigue environments and will continue to be.
This very fact means that nitinol is challenging our anatomical knowledge base. Physicians are placing stents in fatigue environments that are, at best, poorly understood and often unanalysed by engineers. Again the SFA provides a wonderful example of this. Just five years ago, this was considered to be a largely static vessel. Only after nitinol stents were implanted did physicians begin to understand its complex dynamics.
It is important to note that a fracture does not equate to device failure. Studies have shown that a fracture in some designs leads to a high probability of clinical failure, while fractures in others do not. One could even argue that some programmed breakage is a good thing, relieving stresses at the locations that are interfering most with native vessel movement. In fact, fatigue testing as a whole is being reassessed, to incorporate newly found deformation modes and testing to failure, in the hope of finding better predictors for failure rather than simply trying to prove that nominal conditions are fatigue safe.
BIOCOMPATIBILITY AND CORROSION
There is seemingly endless discussion on the subject of nitinol’s nickel content (about 50 atomic per cent). There is no doubt, of course, that nickel on its own can pose a health threat, but nitinol forms a protective TiO2 barrier, all but preventing nickel from being released into the body.
Early investigations into nitinol’s corrosion behaviour were unfortunately inconsistent. In fact, many early investigations were performed on improperly prepared and highly contaminated material. Explanted nitinol devices have also been reported to exhibit pitting, although later studies have shown this to be a result of improper surface preparation and the way tissue was removed from the explanted devices. It is now well established that when devices are properly electropolished, they exhibit nickel release rates below those of stainless steel.
Nevertheless, a preliminary correlation between stent restenosis and nickel allergies has been indicated, causing many researchers to search for a superelastic alloy that contains neither nickel nor other problematic elements. The only candidate systems at the moment are the beta titanium alloys. Although researchers are constantly reinventing concoctions of beta-stabilising elements, to date none have performed better than the original Ni-Nb, which has properties far inferior to nitinol.
ALLOY PURITY
There are essentially two methods of melting nitinol in widespread use: Vacuum Induction Melting (VIM) and Vacuum Arc Remelting (VAR). The relative merits of the two approaches continue to be hotly disputed – with both sides claiming superior fatigue life. Proponents of VIM point out that it results in smaller oxide inclusion sizes, while advocates of VAR stress that this method avoids carbide inclusions (introduced by the carbon crucibles used in VIM).
In fact, there is no objective proof that one method is better than the other, in terms of either fatigue or corrosion. Ultra-high purity nitinol, low in both carbon and oxygen, has recently become available, with no carbides and a sharply reduced oxide content. While the purity and inclusion levels are unarguably better, definitive proof that fatigue life is improved awaits the outcome of further studies. The upcoming SMST-2006 conference promises to report on these studies (see www.smst.org for more information).
PROMISING FUTURE
Progress is taking place in all of the above areas, but none of this is as important as simply improving our understanding of human anatomy. The use of conventional materials to dominate the native anatomy requires an understanding of the properties of the device, but nitinol’s physiological compatibility makes it imperative that anatomy and physiology are also understood.
A consortium of industrial stent producers called ResiStent is actively working to define the movement of the SFA and other peripheral vessels with the hope of developing common, intelligent fatigue requirements and test methods. (See www.sri.com/psd/fracture/stents for more information.) There is a great opportunity for the medical devices industry to define requirements and standards before the FDA and other regulatory agencies step in and mandate requirements – the FDA supports this approach to self-regulation. The nitinol community should rise to the challenge and work together to make sure it is governed by sensible and meaningful standards set by people that understand nitinol’s complex behaviour.
RADIOPACITY
Finally, a few comments on radiopacity, a desirable quality in stents as well as other applications. Again, much of the medical community has drawn some incorrect conclusions. Nitinol is actually very similar to stainless steel in its radiopacity, even although it has a reputation for being far less visible. Still, greater opacity is required, although few options are available for enhancing the radiopacity of nitinol. The radiopaque coatings and cores used to enhance the radiopacity of conventional materials generally cannot survive the deformations to which nitinol is subjected.
Gold and other noble metals dramatically accelerate corrosion and nearly all alloying additions change nitinol’s properties, even when added in small amounts. To date, designers have had to resort to attaching galvanically acceptable markers in areas that do not deform, or using platinum or palladium alloying additions. This remains an active area of research.





