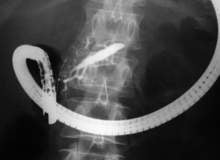
An increasing incidence of pancreatic cancer has spurred the use of biliary stents in the global non-vascular stent market. Biliary metal stents are now being used with percutaneous procedures for the treatment of biliary strictures, a shift that is putting the market in good stead for growth in coming years.
Another important factor pertaining to the global biliary stent market is the use of these stents for indications other than bile duct blocks. Biliary stents are increasingly being used for the treatment of peripheral vascular diseases because of their cost effectiveness and the lack of clinical evidence proving the devices unfit for such uses, according to a recent report by analyst firm GlobalData titled ‘Biliary Stents: Off-Label Use to Drive Growth’.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Biliary stents and the gold treatment
Bile duct strictures occur in a benign and a malignant form. Malignant ones are more common and occur as a result of the onset of pancreatic cancer. In general, most benign strictures are caused by post-operative effects.
Bile duct strictures may be asymptomatic but, if ignored, can cause life-threatening complications such as ascending cholangitis, liver abscess and secondary biliary cirrhosis. Data from many large series of patients in the US have revealed that the incidence rate of major bile duct injury is 0.2–0.3% after open cholecystectomy and 0.4–0.6% after a laparoscopic cholecystectomy.
The exact prevalence of overall strictures is not clear due to lack of long-term data collection; however, more than 30,000 new patients with pancreatic cancer and 4,000 new cases of bile duct cancer are diagnosed in the US each year, most frequently in the older population.
A biliary stent is essentially a plastic or metal tube inserted into a bile duct to relieve a bile duct stricture. The use of metallic stents is the gold standard for treatment of such conditions. Elgiloy, a cobalt-based alloy, is employed in some stents.
The two most common methods used to place a biliary stent are endoscopic retrograde cholangiopancreatography (ERCP) and percutaneous transhepatic cholangiography (PTC). Traditionally, surgical removal of biliary strictures was the mainstay of treating strictures. Slowly the trend shifted towards the use of single or multiple plastic stents with better endoscopic and percutaneous delivery techniques. Compared to surgical removal, insertion of plastic stents was better tolerated and also prevented post-operative strictures.
Plastic stents vary in calibre, length, material and configuration, depending on the design and intended application. Plastic stents, however, proved to be susceptible to early stent occlusion. This early stent occlusion is attributed to internal adhesion of bile protein and bacteria to the plastic material.
Teflon and two-layer stents are also being used in recent designs and are aimed at improving stent patency by decreasing bacterial and protein adhesion. The entrance of self-expanding metal stents (SEMs) to the market added the promise of overcoming early occlusion problems inherent to plastic stents. For one, the larger diameter is observed to have prolonged stent patency when compared to plastic stents. Most SEMs are made of Nitinol, a superelastic nickel-titanium alloy with thermal shape memory which allows it to reassume a predetermined shape through heating.
Off-label use – an industry concern?
Biliary stents have been approved for use in the draining of bile ducts but there are reports of off-label use of these stents for propping up clogged arteries. Though there has been no long-term hard data proving that use of biliary stents for clogged arteries is unsafe, reports of adverse events are high with off-label use.
An estimated one million people were treated with biliary stents for clogged arteries during 2003 and 2006. In the same period nearly 88% of the 561 problems reported to the US Food and Drug Administration (FDA) involving biliary stents occurred in off-label use.
The primary issue with off–label use of biliary stents is the approval process. Biliary stents undergo the 510 (k) or class II approval process, which has minimal regulation and testing compared to class III devices.
Scientific and other companies in this market have already received letters from the FDA relating to the off-label use of biliary stents. Even without off-label use, increasing awareness of biliary stents coupled with an increasing incidence of bile duct blockages is expected to boost sales in the global biliary stent market.
The FDA has issued warning letters to all manufacturers of biliary stents to refrain from marketing or pushing off-label use. At the same time, knowing that 90% of biliary stents are used in the circulatory system instead of the bile duct, the FDA continues to approve biliary stents with minimal requirements as a class II device.
Many companies, including stent giant EV3, have started clinical trials to prove the safety of biliary stents in the circulatory system. However, industry experts and some physicians still believe that the biliary stent is a device made for patients suffering from pancreatic cancer with low life expectancy and should not be used for patients with normal life expectancy.
With the lack of clinical trial outcomes proving the safety of biliary stents for use in arteries or veins, the FDA will be forced to enforce more stringent laws relating to the use of biliary stents. This could have an effect on the market in the US and could cause up-classification of biliary stents as a class III device.
The increasing prevalence of pancreatic cancer in the developed countries and the unregulated use of biliary stents for off-label use in developing nations like India, China and Brazil, however, should keep the volume sales of biliary stents growing.
The future of stents
The US constitutes 38.5% of the global market for biliary stents. Japan comes in second with a 30.8% share and the global biliary stent market was valued at $70m in 2008. Driven by increasing cases of benign strictures, this market is expected to grow at a CAGR of 7.3% during 2008 and 2015 to reach sales of $114.4m in 2015.
Research underway could help the market overcome any US loss. Metal stents, for example, have been in use for the treatment of bile strictures but frequent clogging, requiring repeat procedures, has made some reluctant to go for this option. The possibility that clogging occurs from the contents of the intestines backflowing, also known as reflux, is also being studied. The future of biliary stenting may stem from this concept.
Studies on stents that prevent reflux, known as anti-reflux biliary stents, are already under clinical trials. These stents promise to reduce the repeat procedures needed with ordinary metal stenting of the bile duct.
The Dua Anti-Reflux stent approved by the FDA in 2007 is one such model promising to deal with problem of refluxing. Clinical trials have already proved the safety and efficacy of anti-reflux stents over that of open stent systems for bile ducts. Another future prospect that could well become the gold standard for treating biliary strictures is fully bioabsorbable stents. These stents, already in trials for use in arteries are expected to bring the same advantages for use in the bile duct.
Despite problems with off-label use, innovation will still occur in the space, especially while there is strong demand for the outcomes of biliary stents in medicine. The future looks bright around the world, even in the US where trials will be underway to prove the worthiness of use in other medical procedures.
The report is available to purchase via GlobalData’s Report Store (http://www.global-market-research-data.com/)





