In July 2019, US President Donald Trump signed an executive order designed to streamline America’s overburdened kidney care and transplant system. The policy aims to improve kidney care by increasing the rates of living and deceased organ donation, improve preventative care and introduce new treatments – including at-home dialysis.
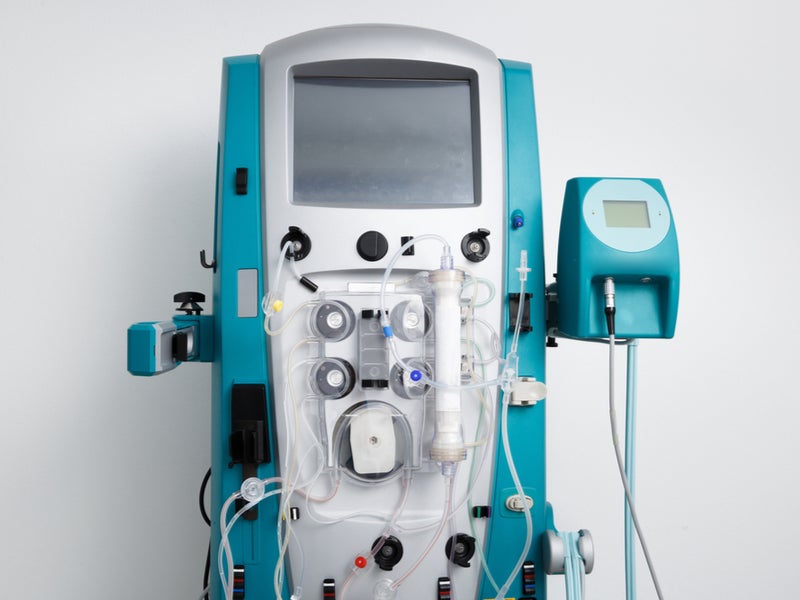
End-stage kidney disease patients require dialysis to clear their blood of waste and excess fluid, meaning they must spend three to five hours hooked up to a machine which filters impurities from the blood three times a week.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Having this procedure carried out in a clinic can clearly have a significant impact on a patient’s quality of life. As well as being hugely time-consuming, dialysis can cause exhaustion, itchy skin and muscle cramps.
“Home-based dialysis, including home haemodialysis, improves patients’ quality of life and will become more popular,” says GlobalData medical analyst Tina Deng. “According to the National Kidney Foundation, patients who have more frequent dialysis, during the day or overnight, have better health outcomes than those who visit an outpatient centre three times a week.
“Home haemodialysis also gives patients opportunities to control the place and timing of conducting dialysis, making it even more appealing to patients in rural regions who try to avoid long commutes to dialysis centres.”
The global dialysis equipment market is predicted to register a compound annual growth rate (CAGR) of 4.8% and an overall valuation of $23.6bn by the end of 2028, and leading its development are innovative new home dialysis machines.
New players enter the at-home dialysis market
CVS Health recently entered the arena with a clinical review of its new home dialysis system, which would allow patients with end-stage kidney disease to have more frequent dialysis.
Patients enrolled on the CVS trial are expected to undergo dialysis every other day, rather than three times a week, for around six hours a day. This significant increase in time spent on dialysis is hoped to generate better overall outcomes for patients. CVS is planning to enrol up to 70 patients in up to ten medical centres across the US for a 16 – 18 month study, with plans to offer home dialysis services as early as 2021 if successful.
The system is contained in two cabinets the size of small countertop fridges, operated through a software program on a tablet computer. Patients will be trained in how to use the system by a nurse for six weeks, then operate it independently for a further six.
In the UK, Quanta Dialysis Technologies has raised $48m to fund the commercial launch of its SC+. This home haemodialysis machine is designed with intuitive operation in mind, making it easy for patients to operate at home without the extensive training of a clinician. The system moves the fluidics circuit onto a single-use disposable cartridge, minimising the need for disinfection and descaling.
Accessibility issues for at-home dialysis
However, regardless of the exciting developments in home haemodialysis, the technology still remains inaccessible to many patients.
“Patient demographics, reimbursement policies, cost issues and physician comfort levels have restricted broader use of home haemodialysis,” Deng says. “Because of the complicated procedure, home haemodialysis is only appropriate for a small number of usually younger patients. Older dialysis patients often suffer from more than one chronic disease, which makes it difficult to perform haemodialysis at home.”
It’s not just health issues that can bar patients from home haemodialysis, Deng adds. Some patients simply won’t have the room in their home to accommodate a dialysis machine. And in the US in particular, health insurance for home haemodialysis is not sufficient to cover the costs of purchasing and operating the machines and supporting the visits of home health nurses.
More than 726,000 Americans have irreversible kidney failure and need dialysis or a transplant to survive, with more than 500,000 of them receiving the life-saving treatment at least three times a week. The average wait time for a kidney transplant can be three to seven years, meaning access to home haemodialysis can mean years of increased freedom and quality of life. With more and more new home dialysis machines in development, only time will tell whether US health insurers will start to include more of them under their patient’s plans.





