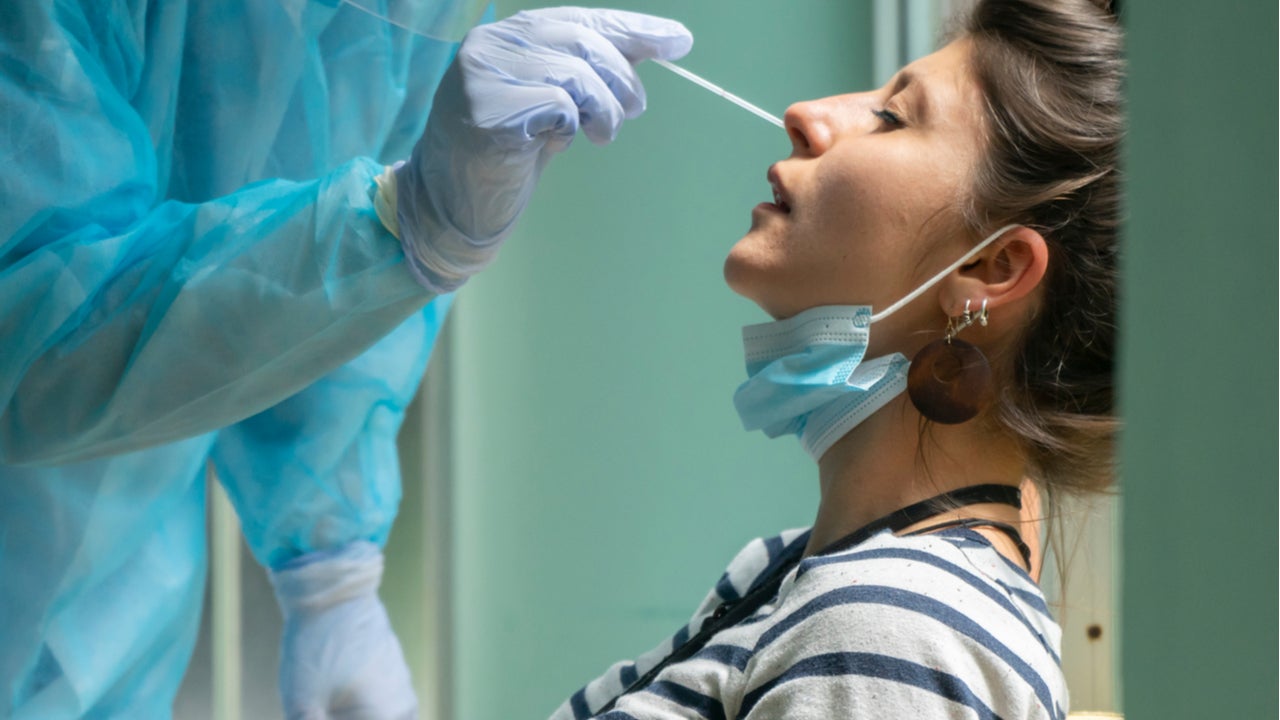
The Importance of Mass Testing in the Covid-19 Pandemic
The way Covid-19 cases are counted in the UK has changed since the start of the pandemic. It’s switched from a focus on people with symptoms and a positive polymerase chain reaction (PCR) test result to including asymptomatic people with a positive PCR test result, and then widened to include results from lateral flow tests (LFTs) as well.
Of course, testing for disease during a pandemic is a sensible measure in keeping the virus controlled among the population. But researchers disagree about how much asymptomatic people are contributing to the spread of Covid-19, and thus how useful – or even harmful – mass testing of asymptomatic people can be.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Some believe asymptomatic or pre-symptomatic carriers could be contributing to a sizeable portion of transmission events, as they’re more likely to be out in the community and interacting with others than people who know or suspect they have Covid-19 and are staying at home. Others, however, note that since they’re not coughing or sneezing in the way a symptomatic Covid-19 patient would, they may not be spreading viral particles as widely.
Research early in the pandemic suggested that the rate of asymptomatic Covid-19 infections could be as high as 81%, but a meta-analysis of 13 studies last month put this statistic closer to 17%.
“What we do know is that the time window when you’re infectious but haven’t got symptoms yet, or are infectious and are never going to get symptoms, is relatively short – a matter of one to three days based on current knowledge,” says public health consultant and University of Bristol senior lecturer Angela Raffle. “That’s why people are now starting to say it would need daily home testing, to pick people up in that important time window.”
Searching for asymptomatic people “like searching for needles in haystacks”
The UK Government is currently operating on the assumption that asymptomatic spread is a significant factor in the pandemic, and aiming to test large numbers of people to identify these asymptomatics and isolate them. The government is planning to expand regular asymptomatic testing to several groups, including: NHS patient-facing staff, care home staff and residents, home-visit carers, people visiting relatives in care homes, food processing staff, prison staff and inmates and vaccine distribution workers.
The government is also piloting rapid testing in schools, colleges and universities. It is also allowing any local authority in Tier 3 of it’s England-wide Covid-19 restrictions to enter into a community testing programme and is working with devolved authorities to expand this across the rest of the UK.
But following a Covid-19 mass testing trial in the city of Liverpool, a letter from five public health experts to local MPs criticised the initiative to test asymptomatic people, saying: “searching for symptomless yet infectious people is like searching for needles that appear transiently in haystacks.”
Raffle says: “The whole thing has kind of gone back to front. Medical testing devices are way less regulated than pharmaceuticals. There’s no way that if somebody says ‘I’ve come up with a vaccine, I’ve tested it on 30 people in ideal circumstances and I think it’s really good’ that we would spend billions on it and start using it. But in effect, that’s what’s happening with tests.
“If we were approaching this in a ‘doing the best for the public with public funds’ kind of way, we would be doing the field tests and working out how much it could decrease transmission before we spent billions. At the moment we’re in a bit of a messy situation because it’s being rolled out anyway and we haven’t had the field studies. The government’s already spent tens of millions on these tests anyway, so they’ve got warehouse loads of them, and they just want to get them used.”
False negatives and false positives pose huge risks
No screening tool is infallible, and all will carry a risk of false negative and false positive results, even if it’s only small. The sensitivity and specificity of both the PCR and LFT devices being used in the UK to diagnose Covid-19 have been the subject of much debate, which is the key reason experts are concerned about mass testing. Both methods appear to have low false positive rates, but when it comes to population screening low does not mean negligible, and false positives could become a significant problem.
Biostatistician Professor John Deeks has argued that even if the Covid-19 tests being used had a very good specificity of 99%, meaning only 1% of healthy people could inadvertently be told they were infected, mass testing a population the size of the UK’s could result in over half a million people wrongly being told they had to self-isolate, along with their close contacts. While for some members of the population, being ordered to self-isolate is little more than a lost two weeks, for others – low-paid essential workers who will not receive sick pay, for example – the impact could be devastating.
False negatives are an even larger concern. Preliminary data suggests that the LFTs currently being trialled in the UK have returned very few false positives – 99.68% of people who didn’t have the virus received a negative result – but considerably more false negatives. Just 76.8% of people who have the virus received a positive result. While PCR swab tests are thought to deliver very few false negatives under ideal sampling conditions, many of these tests are now being self-collected or collected by untrained staff, meaning we don’t have reliable data on how many false negatives they may be delivering.
If someone who has Covid-19 tests negative, there’s a risk that they’ll go out into the community and spread the disease further. Furthermore, negative results may lull uninfected people into a false sense of security and prompt them to engage in more risky behaviour while they believe they’re highly unlikely to have the disease.
Iceni Diagnostics may have found a solution
There’s another issue with PCR and LFT tests in general – they can only detect the presence or absence of viral RNA in a sample, but not whether that virus is live and capable of spreading. This means that a person may test positive because the swab is picking up viral debris from a recent past infection.
British firm Iceni Diagnostics has now developed an LFT that is designed to reveal if live, intact virus is present, rather than just viral genetic material. The technology works by detecting the way the virus interacts with the sugars that surround human cells, rather than searching for the virus itself.
Iceni Diagnostics co-founder and CEO Dr Rob Field says: “What is clear is that the genetic material from the virus can hang around well after an individual is infectious. Our test is very much more focused around trying to detect the effects of the infectious agent, not bits of protein or nucleic acid that have come from the agent.”
If the assay proves successful, it could change the way mass testing tackles Covid-19 in the UK. By confirming whether or not a person has actively infectious Covid-19, rather than that some form of viral RNA was picked up on a swab when they had their test, public health authorities can be more confident that people being ordered to isolate really do need to do so.
The test could also help to inform our understanding of whether the people being classed as asymptomatic are infectious or not in wider studies. For example, if enough people without symptoms were to test PCR positive but Iceni LFT negative, it could indicate that they aren’t actually at risk of spreading the disease. On the other had, if the Iceni test came back positive too, it would show that they are capable of spreading the disease even if they don’t feel unwell.
Iceni doesn’t yet have any data on the sensitivity or specificity of its assay, but it is now beginning to trial it in care homes. Cambridge Clinical Laboratories will be running a clinical evaluation of it over the coming weeks. The assay is also undergoing trials at Norfolk & Norwich University Hospital Laboratories and testing at Porton Down has been commissioned by Public Health England.
If Iceni’s test were to be incorporated into the UK government’s scheme, Field says it would function best as a first port of call. It’s a rapid test that can indicate the presence of infectious Covid-19 within minutes, rather than needing to be sent away and analysed in a lab like a PCR test, and it’s also much cheaper. If it indicated active infection, only then would it be followed up with a PCR for final confirmation.
“One of the problems with the whole ‘Operation Moonshot’ sort of idea is it’s tipping towards the idea that there’s a single silver bullet, one assay that can do everything,” Field says. “I think there’s a real risk that we’re going to get caught in a trap of looking for something that’s perfect when something that’s very good will save tens of thousands of lives. We’re much closer to very good as a collective of different integrated diagnostic approaches. We shouldn’t be looking for a single solution for everything, because we could be waiting too long and too many people will die in the meantime.”





