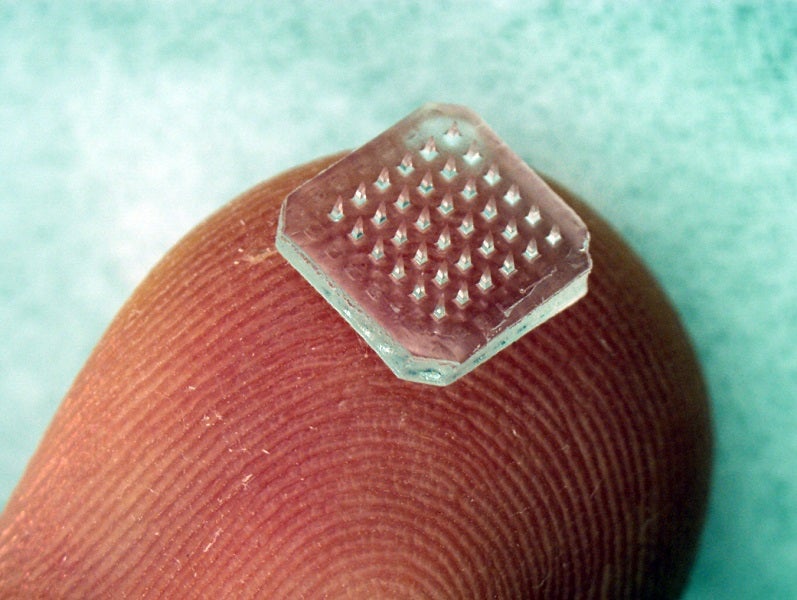
Thinner than a human hair, microneedles are often made from a hydrogel forming substance similar to the material used to manufacture soft contact lenses. Remaining hard in a dry state so that they can penetrate the skin, microneedles rapidly take in fluid from the puncture site and swell, forming a jelly-like material. It’s through this virtually painless needle injection which medicines can be delivered into the body, or biomarkers can be picked up for monitoring purposes.
The needles can also be manufactured as solid, coated or hollow, depending on their intended use. Solid microneedles can deliver drugs into the skin after perforation, while coated microneedles have a layer of medicine pasted over them which is then released into the body. Hollow microneedles allow drugs to be injected directly into the skin through holes in the needles.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Very few microneedle products have reached the mainstream, in part due to the multidisciplinary research and development (R&D) challenges which present themselves in device development. However, this is an area of medtech with significant potential.
Microneedle patches offer breakthrough drug delivery opportunities, enabling the supply of medication to otherwise difficult-to-reach organ sites. The very nature of the needles means they are able to increase medical accessibility to the intradermal capillaries of the lymphatic system, the network of vessels through which lymph drains from the tissues into the blood. This provides an advanced treatment delivery option for patients with diseases of the lymphatic system, such as metastatic melanoma.
The shallow penetration of the microneedle patches also means they’re well suited to deliver treatments to localised skin problems, including certain forms of skin cancer.
Innovators hope to see painless needle injection replace standard syringes
Picofluidics, a life sciences organisation based at Cardiff University’s medtech incubator, is now preparing to go to market with its microneedle product.
Working with scientists from Coventry University and backed by funding from Innovate UK, clinical trials have now confirmed the viability of Picofluidics’ plasma treatment technology, which enables the cost-effective production of microneedle patches.
Picofluidics founder and managing director Dr John Macneil said: “This milestone has been reached after many years of laboratory work developing a specific type of microneedle that can be produced for approximately one-tenth of the cost of those currently on the market. We are now looking to collaborate with partners to commercialise our technology and roll out the benefits to patients.
“We then expect our microneedles to start replacing standard syringes in the delivery of some medicines. Aside from being a more comfortable option for patients, our microneedles produce less waste and potentially offer more control over the dose being delivered. It all makes for better treatment and better outcomes for patients.”
Dr Macneil believes there are many potential uses for Picofluidics’ microneedles, from the painless needle injection of medication such as vaccines or insulin, to intradermal fluid removal for diagnostic purposes and the early detection of disease.
Microneedle patches can also be used to deliver analgesics more effectively than current methods. They are able to bypass the inconvenience of slow-acting, short-duration oral doses and fast but mobility-limiting intravenous delivery by being fast-acting, long-lasting and allowing the user to complete day-to-day tasks.
In January 2019, pain medications delivered through coated microneedles manufactured by Zosano Pharma were revealed to have a statistically significant impact on pain freedom and relief of the most bothersome symptoms of migraine. Nearly 32% of patients were pain-free from 2 hours through 24 hours after patch administration and 27% had sustained pain freedom for 48 hours.
Microneedle technology hasn’t been perfected just yet
Despite their significant promise, microneedles have been subject to numerous R&D challenges in terms of user experience and drug delivery.
Concerns have been raised about how a physician can be sure the full dose of a vaccine or drug has been administered when the microneedle is applied. Both hollow and coated microneedles can cause a drug to leak out onto a patient’s skin, either due to a damaged product or improper administration by a clinician, meaning the treatment may not work properly.
This means that, should this painless needle injection become a mainstream method of drug delivery, extensive clinician training could be needed to properly apply the patches.
The fragility of the some microneedles also means that they have a chance of breaking off from the patch and remaining lodged within the skin. While this isn’t a concern with the dissolvable hydrogel form of microneedle, some of the material used to construct solid, coated, or hollow needles – such as titanium – cannot be absorbed by the body and could cause irritation, meaning the supposedly painless needle injection wouldn’t be quite so painless after all.
However, these potential problems are being closely studied and worked around by academic researchers, companies like Picofluidics and Zosano, as well as organisations such as Nissha, which manufactures microneedle products for both medical and cosmetic purposes.
Cardiff Medicentre business incubation officer Dr Justin John, who has closely monitored Dr Macneil’s work, said: “It is always great to see ideas being brought to life, and I have every confidence that in a few years’ time the technology that Picofluidics has harnessed will be in common use throughout the healthcare community.”





