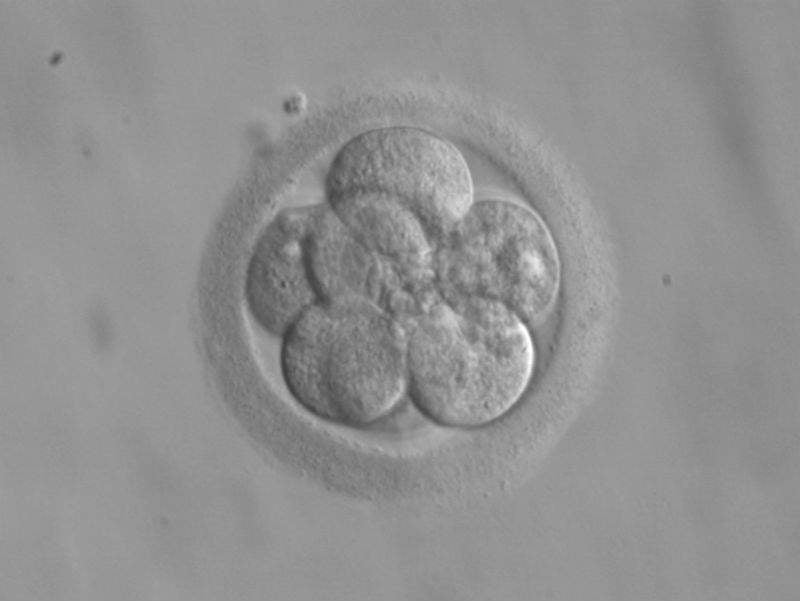
Genetic screening of fertilised eggs for embryo selection during assisted reproduction makes no difference to live birth rates, according to an international study funded by the European Society of Human Reproduction and Embryology.
Results from the randomised controlled trial have been published in Human Reproduction and stress that preimplantation genetic testing for chromosome abnormality (PGT-A) will not increase live birth rates in IVF.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The study began in 2012 and involved 396 women of ‘advanced maternal age’ – between 35 and 40 years of age – as this group were considered the most likely to benefit from preimplantation genetic testing by chromosome screening. Nine centres across seven countries provided treatment to patients who were randomly allocated to treatment with PGT-A or no PGT-A treatment.
One year after the first cycle of treatment, 24% of both the PGT-A group and the control group had given birth. Measured as a cumulative live birth rate, this was the study’s primary endpoint.
A difference was found in the miscarriage rate between the two groups. Significantly fewer patients in the PGT-A group had a miscarriage than those in the control group. This was considered as a secondary endpoint.
A similarity in live birth rates is thought to not only be due to fewer miscarriages in the PGT-A group but also with fewer embryo transfers being required. The authors say this points to “a greater efficiency of transfers with PGT-A”. However, they stress that it has not been confirmed whether benefits of efficiency and reduced miscarriage can sufficiently outweigh the drawbacks of cost and the invasiveness of the PGT-A procedure.
The study’s principal investigator is Professor Karen Sermon from the research group Reproduction and Genetics of the Vrije Universiteit Brussel in Belgium. She said: “There is now a growing consensus that the most important chromosomal abnormalities interfering with implantation are of meiotic origin – that is, they are derived from the egg or the sperm.”
She added that there was “no benefit” of now offering PGT-A to the patient population of this study, especially in cases where only few eggs have been retrieved. She advised that similarly rigorous trials should now be performed in other patient groups.





