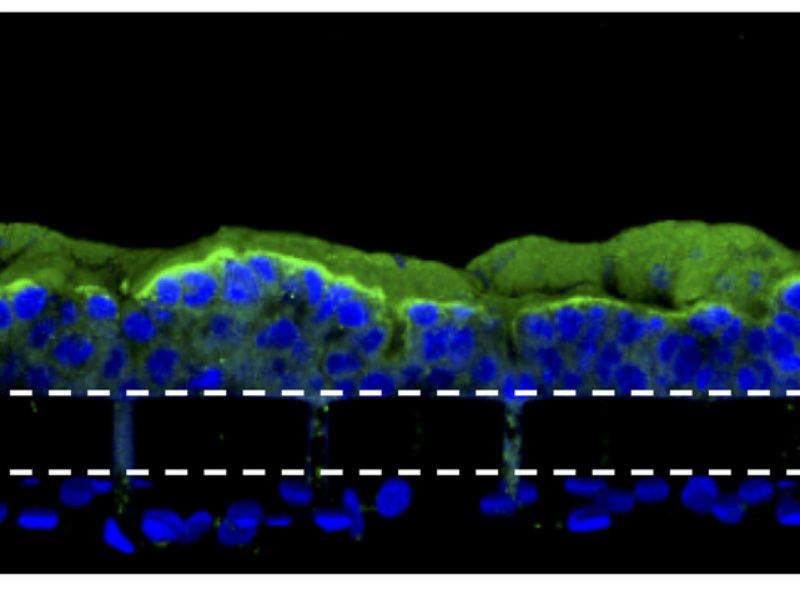
An organ-on-a-chip model of the human gut could offer a better prediction of the effect of radiation exposure on humans than animal testing.
Researchers used the model to demonstrate that intestinal blood vessel cells may play an important part in radiation-induced intestinal injury and confirm that a potential radioprotective drug, dimethyloxaloylglycine (DMOG), can suppress the intestine’s responses to radiation injury.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Scientists from Wyss Institute for Biologically Inspired Engineering at Harvard University, Instituto Superior Técnico in Portugal, Boston Children’s Hospital, and Harvard Medical School collaborated for the study.
Sasan Jalili-Firoozinezhad, first author of the study and graduate student at both the Wyss Institute and the Institute for Bioengineering and Biosciences at IST, said: “When cancer patients receive radiation treatment for a specific organ, other organs are also affected, mostly the bone marrow, the lung, and the gut.
“Radiation in the gut causes the microvilli projections of the epithelial cells to retract, leading to poor nutrient absorption, leakage through the normally tight intestinal barrier, and destruction of the beneficial microbiome. We wanted to see if we could replicate that response in our Gut Chip, and then reverse it with DMOG.”
The research techniques could be used as an alternative to current animal testing methods. Because of the ethical complications of exposing humans to radiation, efforts to identify drugs that mitigate the effects of radiation exposure have been limited to animal studies, which are notoriously poor predictors of how drugs will behave in humans.
An organ-on-a-chip device is a type of artificial organ that can simulate the activities of entire organs and organ systems. The gut chip used in this study is a microfluidic device composed of a clear, flexible polymer that contains two parallel microchannels separated by a porous extracellular matrix membrane. One channel is coated with human intestinal epithelial cells and the other with human endothelial cells which mimic the blood vessel wall.
Cell culture medium is perfused through both channels, and suction is applied to side chambers within the chip at regular intervals to cyclically stretch the tissues, mimicking the peristalsis-like motions that move food through the intestine. Under these conditions the epithelial cells spontaneously form intestinal villus-like structures and surface microvilli that increase the cells’ surface area for nutrient exchange.
The researchers exposed the chip to a radiation dose of 8 Gray, which is known to cause gastrointestinal effects in humans, and observed increases in several markers of cell damage in both the endothelial and epithelial cells: cell death, generation of reactive oxygen species, double-stranded DNA breaks, degradation of lipids in the cell membrane, and loss of microvilli structure, as well as junction disruptions between neighbouring cells and of the mucous membrane that protects the intestinal wall.
The endothelial cells in the blood vessel channel had a stronger response to radiation than the epithelial cells in the intestinal channel in terms of ROS generation, lipid degradation, and DNA fragmentation. In addition, the endothelial cells experienced peak apoptosis levels about 24 hours after exposure, while epithelial cells were most affected at 48 hours. This suggests the endothelium is more sensitive to radiation.
When the scientists repeated the experiment on a chip that only contained epithelial cells, they observed that the irradiated cells did not have the typical radiation response: their microvilli were not blunted, their mucosal barrier was not disrupted, their cell barriers remained functional, and they had lower ROS generation. This suggests that endothelial cells play a key role in the gastrointestinal damage observed in radiation injury.
The team then exposed the gut chip to DMOG, a compound that has been shown to prevent radiation injury in rats. They observed that DMOG pre-treatment significantly reduced apoptosis, ROS generation and lipid degradation in both epithelial and endothelial cells, intestinal permeability, and microvillus injury of intestinal epithelial cells, a result that has never been demonstrated in human tissues before.
“Now that we have successfully tested a potential drug candidate in a human organ system, our goal is to use this chip to identify new radioprotective drugs by physiologically mimicking radiation damage in the gut,” said Jalil-Firoozinezhad.
The team hope their research will lead to a fully personalised body-on-chips model, where cells from a patient could be tested to see which medicines will best protect all their organs from radiation.





