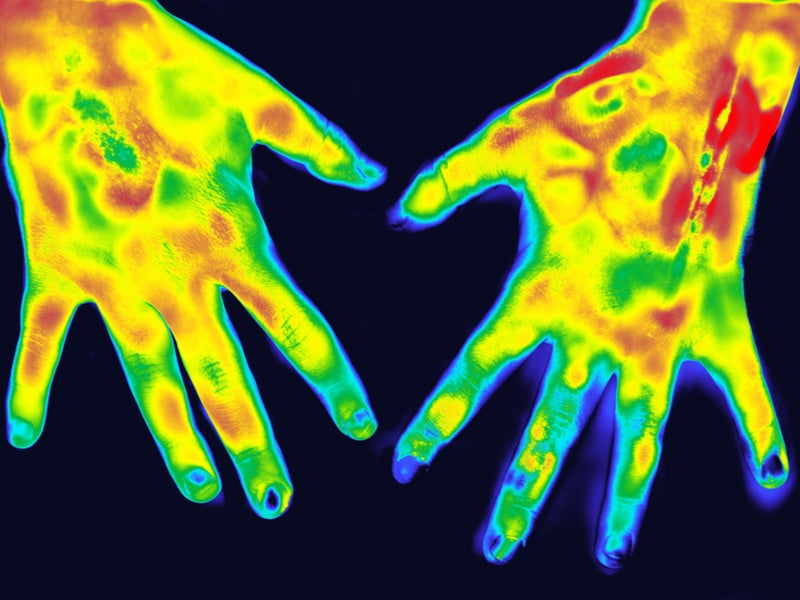
An infrared light test for rheumatoid arthritis (RA) developed by a research team at the University of Birmingham could offer a fast, objective way to diagnose and monitor the joint-attacking autoimmune condition.
The new technique combines 3D digital imaging with infrared spectroscopy to create a 3D image of the blood build-up inside a patient’s hands.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The hand is placed inside a scanner, which creates a 3D model of its size and contours. An infrared beam is then directed through each finger and the amount of light coming through the finger is measured. As oxygenated and deoxygenated blood absorb light differently, the infrared imaging can be used to calculate warning signs of RA such as hypoxia – lowered levels of blood oxygen – and increased levels of blood content, an indication of the inflammation typical of RA.
The researchers infrared-scanned 144 joints from 21 patients with diagnosed RA and compared the results with those obtained by ultrasound and specialist examination. The scanner was able to detect the disease with 88% accuracy. The results have been published in the Journal of Biomedical Optics.
University of Birmingham professors of medical imaging Hamid Dehghani said: “The system we have developed offers a low-cost, objective way of detecting the disease and potentially grading how advanced it is. We hope in time it will enable clinicians to diagnose the disease earlier and offer personalised treatment plans for patients.”
For RA treatments to be as effective as possible they need to be delivered soon after the onset of the disease, but this often comes long before any visible signs of the condition. This means patients instead need to embark on a lengthy process of rheumatology exams, blood tests and x-ray or ultrasound scans before receiving the diagnosis they need, in which time their condition may worsen. The results of the tests also sometimes need to be interpreted, requiring the input of highly-trained clinicians.
Speaking to The Times, Dehghani said: “In the future we are hopeful GPs will not have to send a patient to hospital to be examined by a specialist and scanned with expensive equipment. We envisage they will be able to use a shoebox-sized device in their office. In rheumatology departments it will be a lot quicker and easier for a non-specialist to use an infrared scanner than ultrasound.”
The research team is now investigating ways to miniaturise the scanner and further improve its accuracy.





