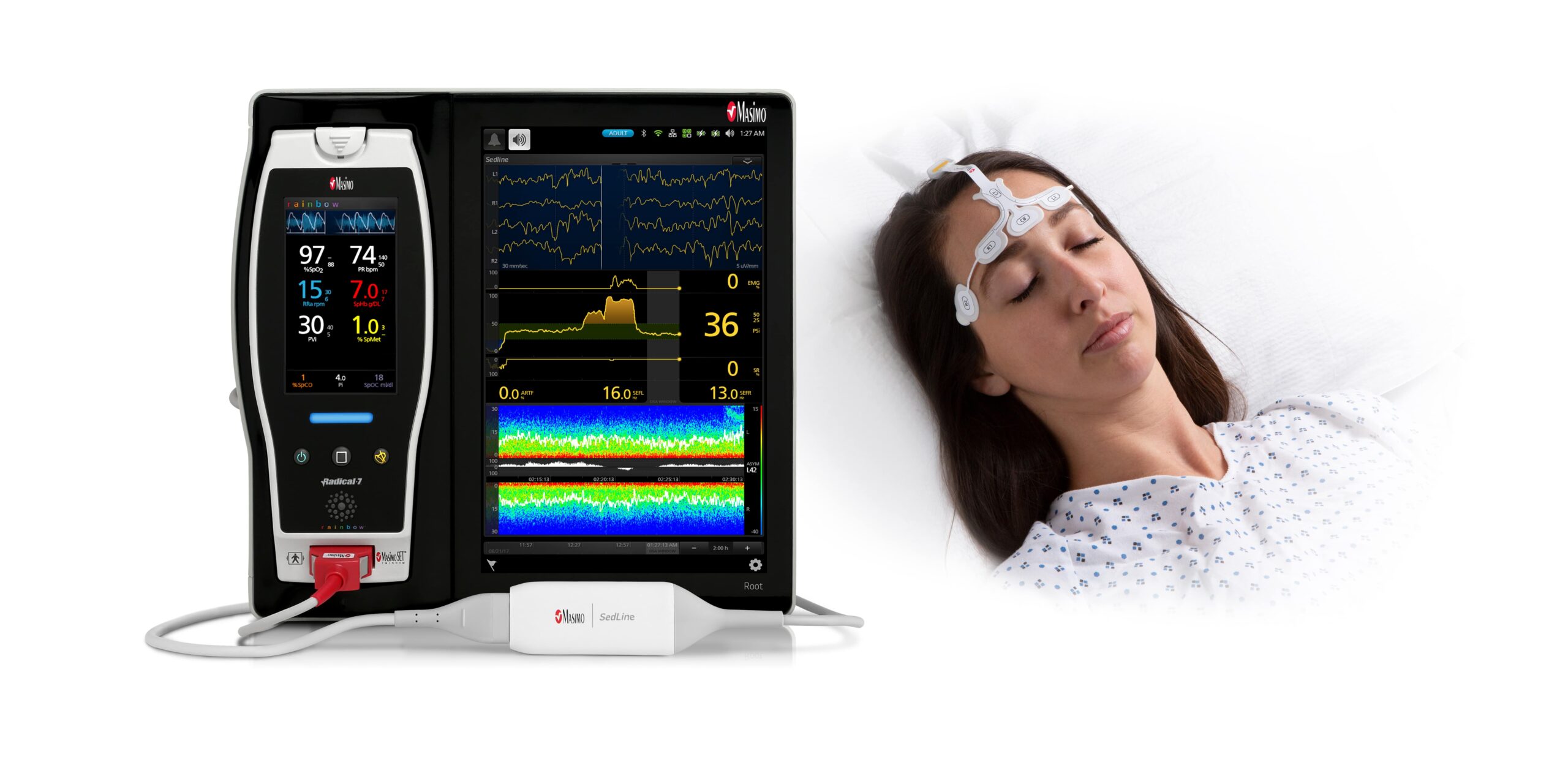
Masimo has reported that two parameters, patient state index (PSi) and suppression ratio (SR), provided by Masimo SedLine brain function monitoring had greater predictability for death 180 days after cardiac arrest, in a study.
The study analysed the ability of these parameters in predicting neurological outcomes and long-term survival in post-cardiac arrest patients admitted to the intensive care unit (ICU).

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
It was conducted in partnership with researchers at the Dongguk University College of Medicine and Yonsei University College of Medicine in Korea.
103 adults were enrolled in the study between January 2017 and August 2020.
These patients all had a non-traumatic out-of-hospital cardiac arrest and were resuscitated after cardiopulmonary resuscitation (CPR). The participants were given targeted temperature management during the ICU stay.
Masimo SedLine was used to continuously analyse PSi and SR from ICU admission to 24 hours after return of spontaneous circulation (ROSC), recorded at intervals of an hour.
The predictive accuracy of the two parameters together or alone as predictors of neurological outcomes was investigated in the study.
Data showed that PSi or SR alone had good predictability for the reduced neurological outcome while the parameters together had increased predictability for death 180 days after cardiac arrest.
Additionally, multimodal prediction utilising the mean PSi and mean SR indicated the maximum area-under-the-curve value of 0.965.
In the study arm, subjects with mean PSi less than or equal to 14.53 and mean SR greater than 36.6 had comparatively increased long-term death rates.
The researchers said: “PSi and SR are good predictors for early neuro-prognostication in post-cardiac arrest patients.”
They added: “The combination of PSi and SR showed better predictability of poor neurologic outcome than did each individual parameter.”
In November last year, Masimo signed an agreement to acquire the entire issued and to be issued share capital of LiDCO Group in a deal valued at approximately £31.1m ($40.1m).





