Researchers at the Massachusetts Institute of Technology (MIT) have developed an in-body GPS system, called ReMix, which can identify the location of ingestible implants inside the body via low-power wireless signals.
The team expects that such implants can be used to track tumours by monitoring even slight movements. In the future, the implants may also help in dispensing drugs to a specific area in the body.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
ReMix is being developed by MIT’s Computer Science and Artificial Intelligence Laboratory (CSAIL) in alliance with Massachusetts General Hospital (MGH).
The in-body GPS system is based on a wireless technology that MIT previously developed to detect heart rate, breathing and movement.
To validate the system, the researchers implanted a small marker in animal tissues. They used a wireless device that reflects radio signals off the patient to track the marker’s movement.
This marker does not transmit any signals of its own. It merely reflects those transmitted by the wireless device. As a result, the marker does not need a battery or any external source of energy.

US Tariffs are shifting - will you react or anticipate?
Don’t let policy changes catch you off guard. Stay proactive with real-time data and expert analysis.
By GlobalDataThe researchers further utilised an algorithm, which can use the reflected radio signals to accurately detect the location of the marker. It was observed that using ReMix, the implants can be tracked with centimetre-level accuracy.
In order to avoid interference from other signals, a diode was used to filter out the skin-related signals.
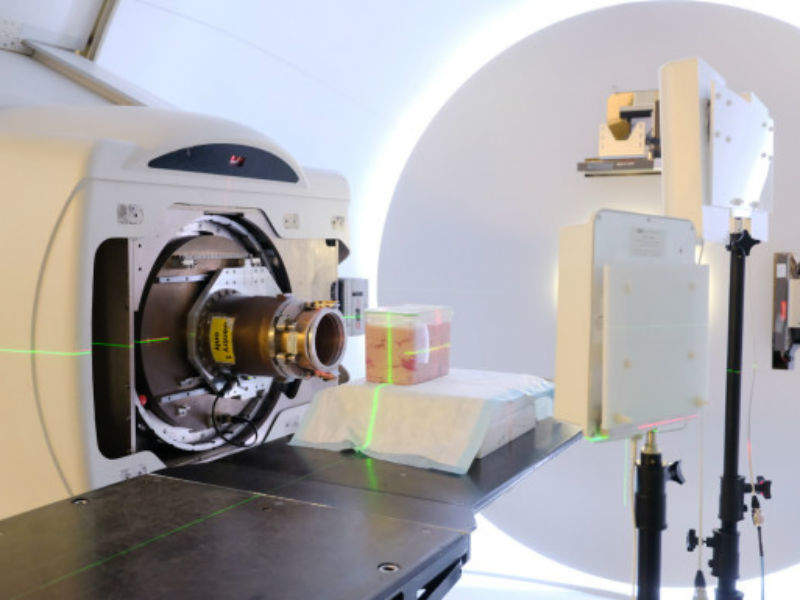
ReMix can be potentially used in proton therapy for cancer treatment, where higher doses of radiation and a high degree of precision are required.
The in-body GPS system is expected to help in pinpointing the location of a moving tumour in real-time, thereby reducing the risk of damaging healthy tissues.
However, further studies are required to improve the system’s accuracy and address any associated challenges.
MIT PhD student Deepak Vasisht said: “We want a model that’s technically feasible, while still complex enough to accurately represent the human body.
“If we want to use this technology on actual cancer patients one day, it will have to come from better modelling a person’s physical structure.”





