Post-mortem scans of injured brains are causing researchers to question the hypothesis that blunt force trauma from traumatic brain injuries (TBI) causes nerve damage.
The scans, conducted by a team including researchers at the New York-based Cold Spring Harbor Laboratory (CSHL), have shown greater signs of blood vessel damage than nerve damage, and could influence how drugs are developed and treatments are implemented for TBI.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
CSHL professor Partha Mitra said: “Nerve damage following traumatic brain injuries has been a majority point of view, and therapy as well as drug development has been targeted towards that.
“The idea is that if the mechanism is actually different, therapeutic intervention may also be different.”
The CSHL team performed close analysis on post-mortem brain tissue using a high-throughput neurohistological pipeline, an assemblage of techniques for labelling and visualising brain slices, which Mitra had developed to study mouse brains.
Scanning the brains in this way provides much clearer images than magnetic resonance imaging (MRI) alone. While MRI can show clinicians that brain damage has occurred, the resolution is limited and it can be hard to discern whether nerve or vascular injury has occurred.
Correlating neurohistological pipeline scanning with MRI scans allowed the team to see the vascular injuries more clearly.
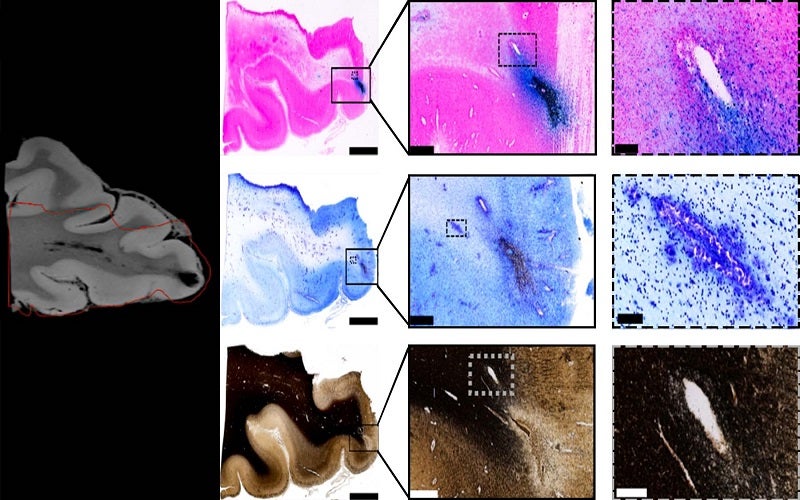
The researchers focused on areas surrounding lesions where trauma had left a physical impact on the brain, which appeared on the MRI scans as black spots.
They then used an iron stain to test for the presence of blood and a myelin stain to test of the presence of nerve fibre fragments in the brain samples. While a significant amount of iron-marked stains appeared in the brain samples in these areas, indicating traumatic microbleeds in the tissue, the researchers did not find any significant nerve damage from the myelin stains.
The researchers concluded that traumatic vascular injury is distinct from nerve damage and could thus be a target for new therapies. They also found that these traumatic microbleeds could often predict future health problems and disabilities for people with TBI, although they could not determine their relationship with acute problems.
The study has been published in the neurology journal Brain.
The team now hopes to conduct research into the underlying causes and effects of TBI for better diagnosis, prognosis, therapeutic targets and patient outcomes.
CSHL worked with colleagues at the National Institutes of Health, National Institute of Neurological Disease and Stroke, University of Maryland, Center for Neuroscience and Regenerative Medicine, and Uniformed Services University of the Health Sciences, which had been studying the brains of deceased patients using MRI.





