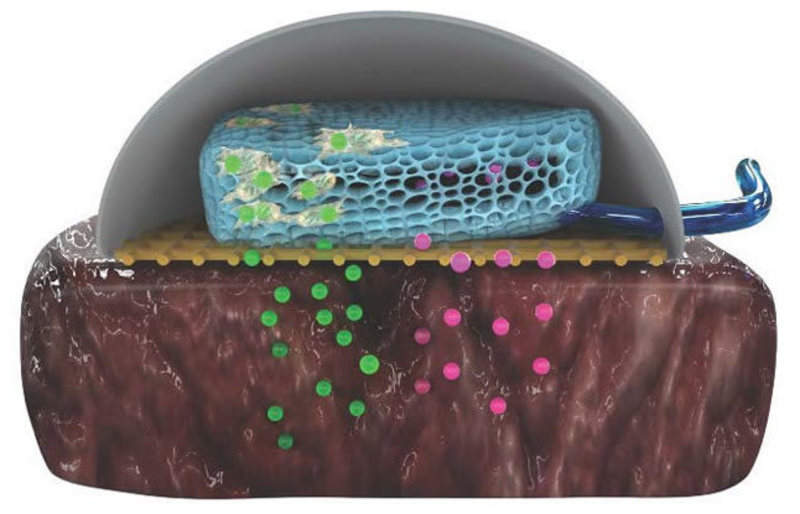
An international team of researchers have developed a new minimally invasive medical device called Therepi that can be placed directly on diseased heart tissue to continuously deliver required drugs, proteins or stem cells.
The team was led by Harvard University, Massachusetts Institute of Technology (MIT) and National University of Ireland (NUI) Galway, among others.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The new implantable tool can be sutured onto tissue and is designed to allow localised, refillable and targeted therapy for the heart.
In an in-vivo pre-clinical study, the device is said to have increased heart function for four weeks after a heart attack, following delivery of cardiac regenerative therapy of stem cells over 28 days.
The device was also able to improve drug efficiency, cut down doses and minimise adverse side effects of therapies that are usually delivered systemically.
Massachusetts Institute of Technology assistant professor Ellen Roche said: “This proof-of-concept study demonstrates that our device can repeatedly deliver drugs and increase retention of cells in proximity to the heart to increase heart function.”
The researchers intend to use the device as a therapy delivery platform in various ongoing studies and will test it as a research tool to gain better insights on localised, replenishable treatment regimens at different pathological sites.
A sponge-like biomaterial has been used to design the patch-like device in order to facilitate storage and release of therapies. The biomaterial can be linked to a port or pump through a tube in case of the requirement for a refill.
Its surface is made of porous polycarbonate membrane, which is permeable and can be altered to be compatible with various sizes of molecules. The pore size can also be changed based on the therapy and time of delivery.
The researchers are working on further optimising the device’s design to support delivery of multiple potential therapies.
They additionally plan to study a combination of the Therepi device with soft robotic extra-cardiac assistive devices in order to enable a mechanical and therapeutic approach for heart disease.





