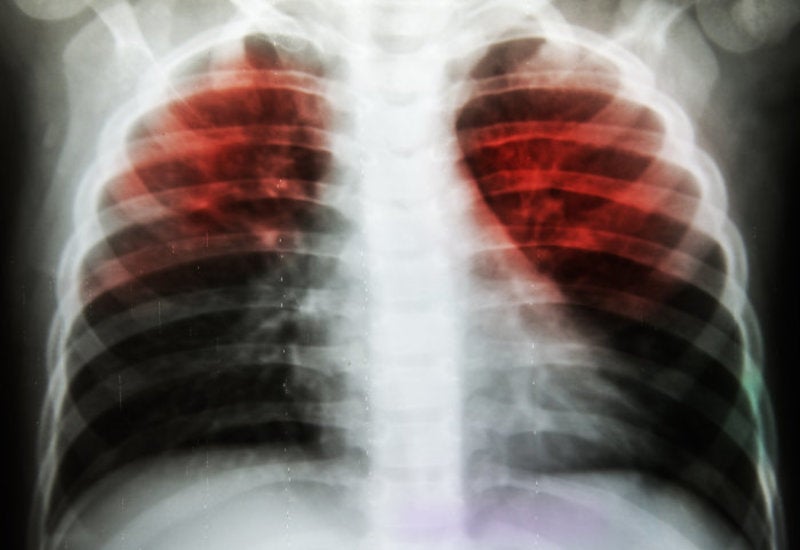
Researchers at Imperial College London in the UK have developed a new second generation blood test for quick diagnosis of tuberculosis (TB).
The new test is also said to enable identification of patients who need further testing and treatment, as well as those who do not and pose no infectious risk to others.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
It consists of TB antigens that are known to be recognised by the immune cells of TB patients.
In addition, the team conducted a study to evaluate the TB tests currently used by the NHS. The tests assessed during the study were two commercially available interferon-gamma release-assays (IGRAs).
IGRAs identify a patient with TB infection through detection of their immune response to TB bacteria using a blood sample.
It was observed that these tests are not sensitive enough to rule out a TB diagnosis in suspected cases.
When compared in 845 patients with suspected TB at ten NHS hospitals, the new second generation test was found to be more accurate, with 94% diagnostic sensitivity in confirmed TB patients.
Existing commercially available IGRA tests are said to possess a diagnostic sensitivity of 67.3%-81.4%.
Imperial College London National Heart & Lung Institute Infectious Diseases chair Ajit Lalvani said: “This study provides definitive, generalisable evidence on the clinical utility of the new test.
“The next step is now to take this new test through regulatory approval so that it can be made commercially available and used in routine clinical practice.”
The researchers believe that the NHS could save more than £2m per year by stopping the use of the existing TB tests, as they are unable to rule out the infection.
Lalvani added: “Existing rapid tests are not recommended for use in patients with active TB because of a lack of evidence that they are clinically useful. But because the clinical need for better diagnosis of TB is so high, they are nonetheless widely used in hospitals.
“Stopping the use of the existing, inadequate tests could save the NHS a lot of money.”
The team added that implementation of new rapid tests could lead to further savings.





