Researchers in Switzerland have developed a non-invasive technique for imaging the carotid artery, which could provide an earlier, more accurate assessment of cardiovascular disease risk than other imaging methods.
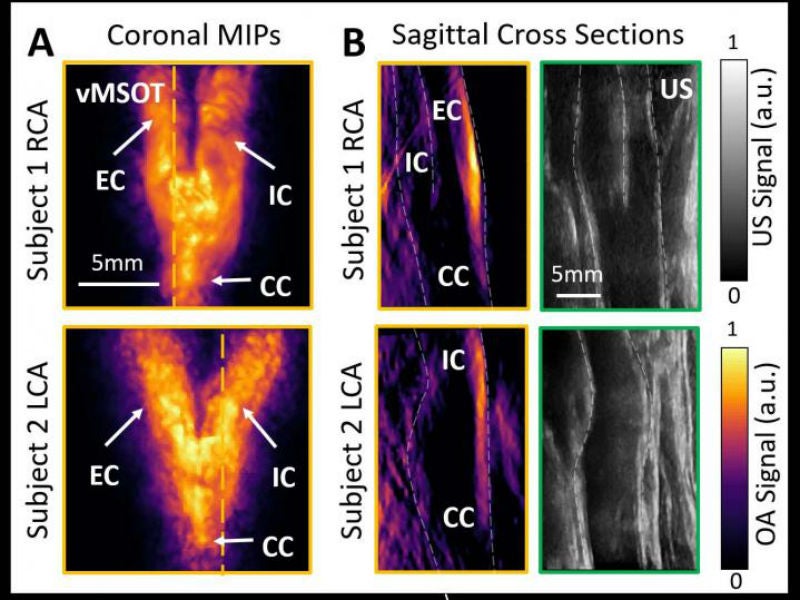
The new cardiovascular imaging technique is called volumetric multi-spectral optoacoustic tomography (vMSOT). A research article detailing the technique has been published in the journal Radiology.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Carotid arteries are located on the left and right side of the neck and bring oxygenated blood to the head. Most ischaemic strokes are associated with carotid artery disease originating in the area where the arteries branch out in a patient’s neck.
Imaging techniques like ultrasound, CT and MRI scans can be used to reveal the extent of narrowing in the carotid arteries but are less helpful in determining the makeup of the plaque itself.
The senior author of the study is Dr Daniel Razansky, director of the Functional and Molecular Imaging Lab at the University of Zurich and the Swiss Federal Institute of Technology. He said: “Rapid characterization of tissue function and molecular composition is limited with these modalities, which commonly results in poor diagnostic accuracy and ineffective treatments.”
Like an ultrasound, vMSOT is performed with a handheld device that is moved around on the neck but vMSOT uses spectroscopy to investigate tissue at a molecular scale, which can provide information about the artery that would not be attainable with other methods. It can also detect lipids, melanin and other disease-related biomarkers early enough to provide a range of treatment options.
Razansky said: “Unlike most other clinical imaging modalities mainly looking at late-stage anatomical manifestations of diseases, vMSOT is capable of sensing specific molecules in tissues without administration of contrast agents.
“In the case of carotid artery disease, assessment of the entire bifurcation area in real time and in 3D is only possible with vMSOT.”
During the study, the researchers used the vMSOT imaging technique on 16 healthy participants and compared their results with participants who had undergone a conventional ultrasound. The vMSOT was said to noninvasively and instantaneously assess the entire bifurcation area of the carotid artery in 3D, which made it less prone than ultrasound to motion-related image-blurring artefacts.
Razansky added: “The developed handheld vMSOT imaging approach holds promise for rapid volumetric assessment of the carotid artery and plaque vulnerability in an entirely non-invasive manner.
“It also has the additional potential for label-free identification and assessment of clinically-relevant biomarkers of carotid artery disease, which helps with early and accurate diagnosis, timely treatment planning and monitoring.”
In the future, the researchers have suggested that vMSOT could be combined with ultrasound to create a more comprehensive characterisation of the carotid artery.
Razansky said: “Given its fast imaging performance, excellent molecular contrast, portability and affordability, I truly believe that vMSOT will soon be routinely used in the clinic. One day, it may even become as popular as ultrasound.”





