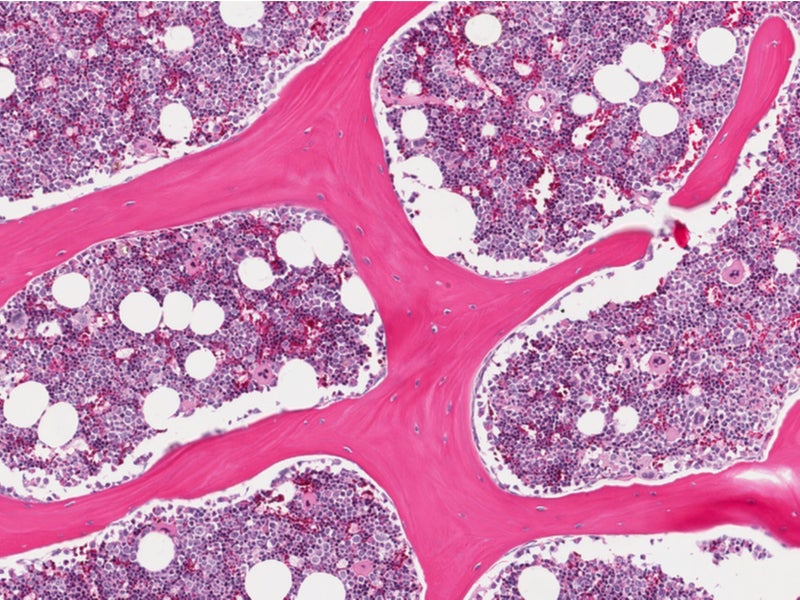
A new research tool that mimics the behaviour of diseased bone marrow has provided a new strategy for understanding the bone marrow disease Shwachman-Diamond syndrome (SDS).
Researchers at Harvard University and Boston Children’s Hospital have used the tool, called the Organ Chip, to build a model system to develop new treatments for SDS. The condition means bone marrow fails to produce blood cells normally, leading to bone marrow failure and an increased risk of leukaemia.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The marrow-on-a-chip has two hollow, parallel channels divided by a semi-permeable membrane. The top channel was filled with blood-forming haematopoietic stem cells from the bone marrow and an SDS patient, alongside stromal cells derived from the bone marrow, including bone marrow stem cells.
The chip was then embedded in a matrix gel to mimic the three-dimensional nature of marrow tissue, and the bottom channel was lined with human endothelial cells to mimic the vasculature of bone marrow.
A liquid medium was then directed through the vascular channel to support the growth of healthy bone marrow cells and their differentiation into many different blood cell types.
Healthy marrow was also applied to a set of organ chips to act as a healthy control group.
The research team was able to see after two weeks that bone marrow on the SDS Organ Chip produced fewer blood cells, especially mature white blood cells, than healthy samples. The blood cell production was impaired in the same manner as it would be in patients.
Animal studies into SDS have been historically difficult to carry out, as inducing SDS in an animal produces very severe disease and causes it to die very quickly. The Organ Chip could provide a viable alternative to research the root cause of and potential treatments for the medical complications found in SDS patients.
SDS National Registry co-director Dr Akiko Shimamura said: “We are going to put patient marrow on the chip, and then flow candidate drugs through the vascular chamber to see if any of the drugs improve the marrow’s ability to produce blood cells. We can then remove the marrow from the chip and study the mechanism by which the drug is working and then develop better or more specific agents.”
The research team also found a previously unknown genetic abnormality of SDS in the Organ Chip. Maturing neutrophil white cells on the SDS chip did not switch on the CD13 gene as they would in healthy marrow.
Pathology reports of SDS patients mirrored the same abnormality in over 50% of cases.



