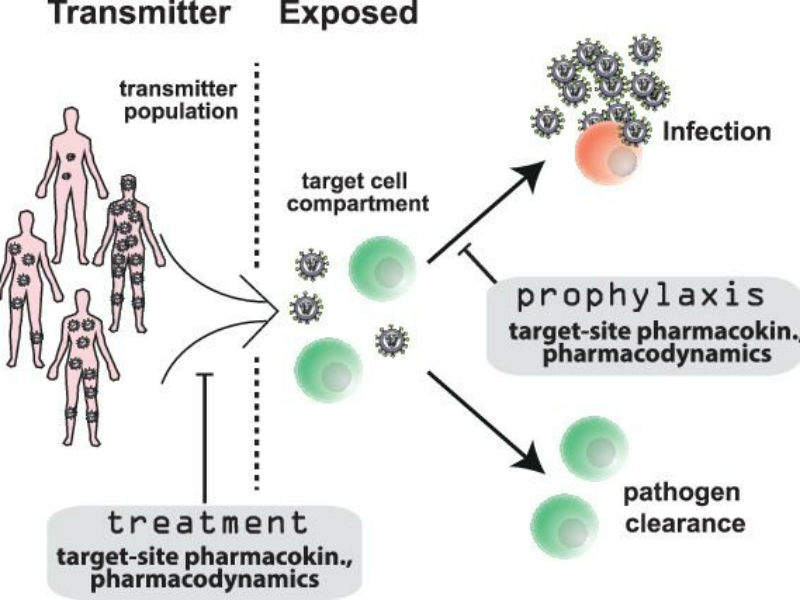
Researchers from Freie Universität Berlin have developed a mathematical simulation tool to predict the efficacy of pre and post-exposure prophylaxis (PrEP) medications, which can help to prevent HIV infection.
The framework of the research, which could help streamline the development of new PrEP treatments, was presented in the PLOS Computational Biology journal by Dr Sulav Duwal, Dr Max von Kleist and colleagues.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
PrEP in the form of Truvada, a two-drug combination, can drastically decrease the risk of HIV infection. However, Truvada has several issues including the fact it is expensive, not 100% effective, and it must be taken once daily which can cause patient adherence issues.
The development of new PrEP approaches is known to be challenged by the inefficiency of testing in patients. In an attempt to address this, the Freie Universität team wanted to build a new mathematical framework to help researchers predict how well new PrEP drugs will work, so that the drugs with the most potential can be identified and optimised for clinical trials.
The mathematical tool integrates a range of molecular factors that affect drug efficacy, including the response of the patient and virus to the treatment. The tool also draws on recent developments in the simulation of stochastic processes to calculate drug efficacy according to drug dosing and drug activity in a patient’s body.
Von Kleist, the senior author of the study, said: “Using the mathematical framework we developed, it is now possible to evaluate the clinical efficacy of any PrEP regimen prior to conducting any confirmatory trial.”
The researchers used the tool to predict that a 50mg oral dose of dolutegravir would be non-inferior to Truvada in pre-exposure prophylaxis but may be superior to Truvada at preventing infection when taken after HIV exposure. They also calculated the blood concentration of dolutegravir required for it to be 90% effective against the sexual transmission of HIV. This information could aid current attempts to develop a long-acting dolutegravir formula.
Von Kleist added: “The cost of PrEP is a major burden to its broad implementation, particularly in sub-Saharan Africa, which is hit hardest by the epidemic. The next step for this research is to evaluate the potential of extremely cost-efficient regimens that are currently neglected in drug re-purposing programs for PrEP.”





