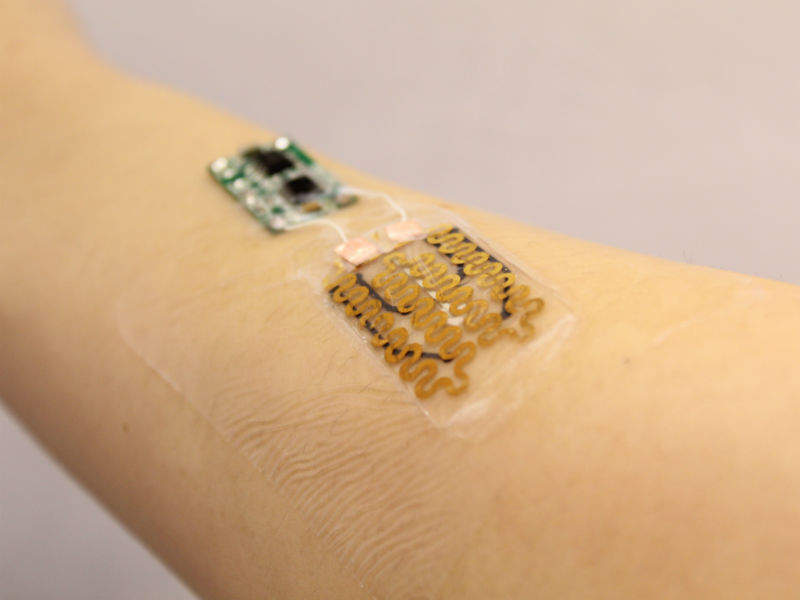
Tufts University in the US has led a team of engineers in developing a prototype bandage that can actively monitor the condition of chronic wounds and deliver appropriate drug treatments to improve healing outcomes.
With the concept of being able to assist the natural healing process, the bandages were designed with heating elements and thermoresponsive drug carriers that deliver tailored treatments in response to embedded pH and temperature sensors that track signs of infection.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
A microprocessor reads the data from the sensors and releases drugs on demand from its carriers by heating the gel. The entire product is attached to a transparent medical tape, forming a flexible bandage that is less than 3mm thick. All the components keep the bandage low-cost and disposable, except for the microprocessor, which is reusable.
The bandages are yet to be assessed in a clinical context but the research has now been published in the journal Small and highlights the engineers’ aim of transforming bandaging from a traditionally passive protective layer into a more active modern treatment.
Non-healing chronic wounds are a significant medical problem. In the US, nearly 15% of Medicare beneficiaries need treatment for at least one type of chronic wound or infection at an annual cost of an estimated $28bn.
Non-healing wound patients are often older, non-ambulatory, and limited in their self-care abilities, despite the condition typically being treated in an outpatient setting. The researchers believe their smart bandages could provide real-time monitoring and delivery of treatment with limited involvement from the patient or caregivers.
Tufts professor of electrical and computer engineering and corresponding co-author of the study Dr Sameer Sonkusale said: “We’ve been able to take a new approach to bandages because of the emergence of flexible electronics.
“In fact, flexible electronics have made many wearable medical devices possible, but bandages have changed little since the beginnings of medicine. We are simply applying modern technology to an ancient art in the hopes of improving outcomes for an intractable problem.”
The smart bandages used in the study combine pH and temperature sensors but Sonkusale and his team have also developed sensors for oxygenation which could be integrated into the bandage. Inflammation of a wound could also be tracked by biomarkers.
Sonkusale added: “The smart bandage we created, with pH and temperature sensors and antibiotic drug delivery, is really a prototype for a wide range of possibilities.
“One can imagine embedding other sensing components, drugs, and growth factors that treat different conditions in response to different healing markers.”
The smart bandages have been created and tested successfully under in vitro conditions. Pre-clinical studies are now underway to determine the in vivo clinical advantages of the product in enabling healing compared to traditional wound care products.





