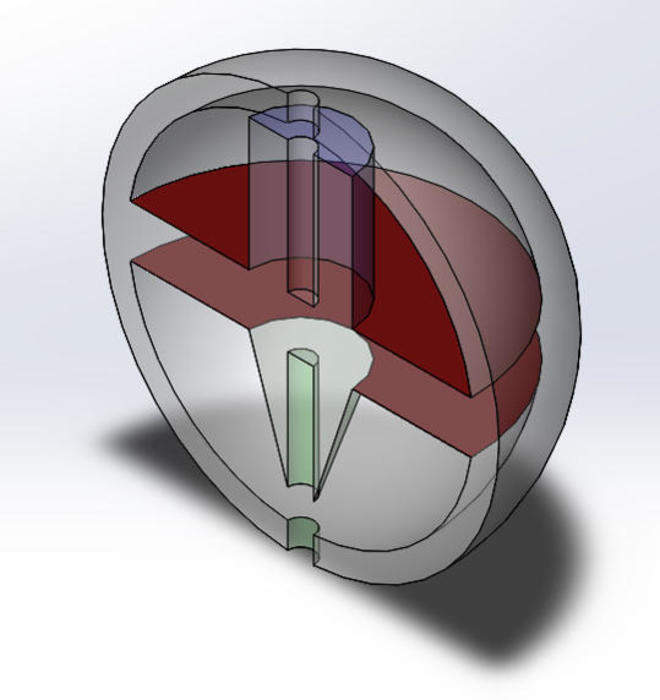
Researchers at the Southwest Research Institute (SwRI) and The University of Texas at San Antonio (UTSA) are developing a 3D printed implant that can deliver a personalised dose of medicine for the treatment of infections, as well as ailments such as arthritis, cancer and AIDS.
Led by Albert Zwiener of SwRI’s Chemistry and Chemical Engineering Division and Dr Lyle Hood of UTSA’s College of Engineering, the project is supported by a grant of $125,000 from the Connecting through Research Partnerships programme.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The implantable device being developed by the SwRI-UTSA team can deliver a controlled, personalised dose of medicine over several weeks.
Zwiener said: “The implant addresses a specific patient’s illness in addition to their medical history and other health issues. We inject this non-invasive device into the body to deliver medicine over a significant period of time.”
The design was created by Zwiener and Hood with UTSA graduate research assistant Priya Jain and incorporates complex geometries to personalise each device to an individual’s ailment and takes advantage of the selective timing and release of the compound.
The device will be created with a specialised 3D printer at UTSA that can print biodegradable materials.
The implant is also engineered to trigger localised immunotherapy for cancer treatments.
According to the SwRI-UTSA team, the localised treatment capabilities of the device can trigger the body to destroy invasive cancer.
Hood said: “In immunotherapy, most strategies employ systemic circulation through an IV line, much like chemotherapy. This can cause issues with immune reactions far away from the intended target. We hope that by delivering locally, we can keep acute effects constrained to the diseased region.”
The implant is ideal for cancer treatment and has been designed to be drug agnostic, which means it can work with any type of drug.





