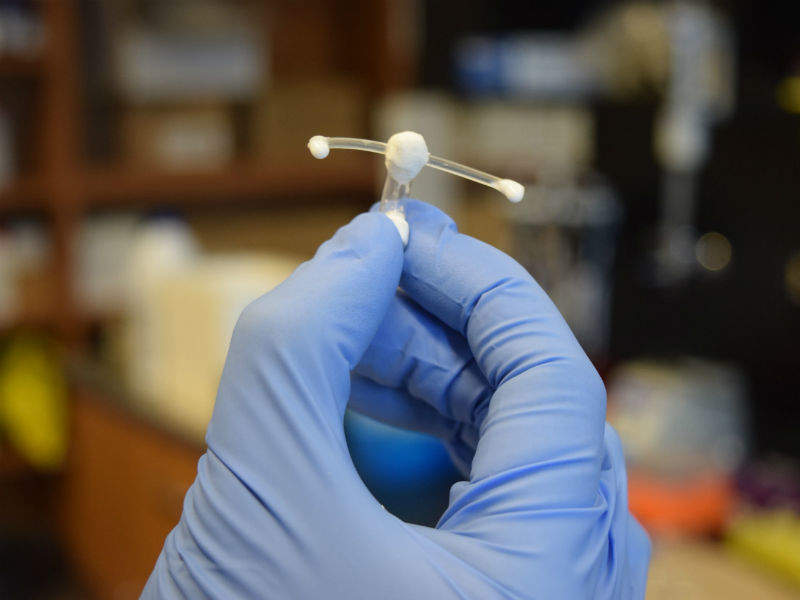
Researchers at the University of Waterloo in Canada have developed a vaginal implant which could protect women from HIV infection.
The implant consists of a hollow tube with two pliable arms attached that work to hold it in place. It contains hydroxychloroquine, which is released slowly through the porous material of the tube and absorbed by the walls of the vaginal tract.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
When tested in an animal model, the researchers observed that the implants resulted in a significant reduction of T cell activation. This meant that the vaginal tract was successfully demonstrating an immune quiescent state.
The implant decreases the number of cells that the HIV virus can target in the female genital tract. Unlike conventional methods of HIV protection such as condoms or anti-HIV medication, it works by taking advantage of a patient’s natural immunity to the virus.
HIV infects patients by corrupting T cells that are mobilised by the immune system when the virus enters a person’s body. When T cells stay resting, also referred to as being immune quiescent, and do not attempt to fight the virus then they are not infected and the HIV virus cannot be transmitted between people.
Waterloo School of Pharmacy professor Emmanuel Ho said: “We know that some drugs taken orally never make it to the vaginal tract, so this implant could provide a more reliable way to encourage T cells not to respond to infection and therefore more reliably and cheaply prevent transmission.
“What we don’t know yet is if this can be a stand-alone option for preventing HIV transmission or if it might be best used in conjunction with other prevention strategies. We aim to answer these questions with future research.”
Ho’s implant was inspired by previous research with sex workers in Kenya. Ho and research partner Keith Fowke of the University of Manitoba, went to Kenya to study why women who had sex with HIV positive clients did not contract the virus. Further research led them to the discovery that these women possessed T cells that were naturally immune quiescent.
Ho said: “Observing this, we asked ourselves if it was possible to pharmacologically induce immune quiescence with medication that was better assured of reaching the point of infection.
“By delivering the medication exactly where it’s needed, we hoped to increase the chances of inducing immune quiescence.”



