Interventional medicine is as much an art as it is a science. While doctors operate based on best practices and clinical evidence, not every possible situation can be covered or studied. In these cases, a surgeon’s intuition and surgical experience is what separates the great from the good, allowing them to come up with an improvised solution that may not have the weight of clinical evidence behind it.
These insights and tricks are then shared among doctors and surgeons to increase the quality and efficacy of medical care across the profession. However, just because a procedure is shared or widely used does not necessarily mean that it is ultimately efficacious.
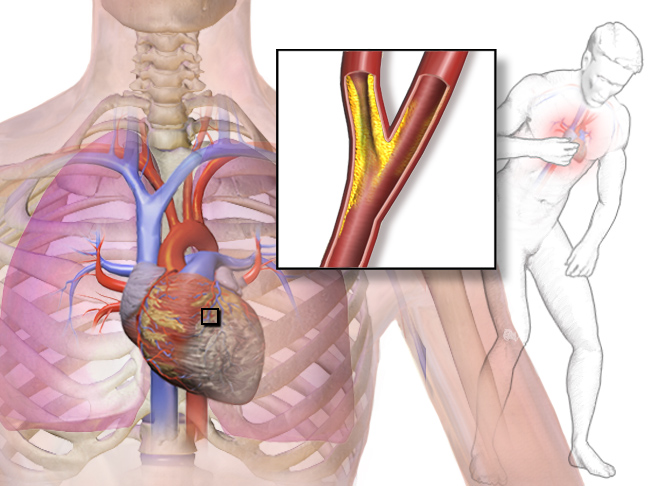
Stable angina has been one of the main indications for coronary stents across the world for almost three decades, ever since artery stenting was first invented. It is widely believed that coronary stents help alleviate the symptoms of angina by widening the affected arteries, thus restoring normal blood flow. As such, it is one of the main treatments for this indication, along with pharmacological treatments or simple angioplasty. GlobalData estimates that stable angina stents costs the US approximately $21.8m a year in device costs alone.
ORBITA trial: the end of stents for angina?
In early November 2017, the ORBITA clinical trial found that coronary stents did nothing to relieve the symptoms of stable angina. ORBITA was a double-blind trial wherein stable angina patients were treated with either actual coronary artery stenting or a placebo procedure. The participants were then followed, and the efficacy of their treatment was assessed by the rate at which they were able to perform strenuous exercise without aggravating their angina. The ORBITA trial found that there was no difference between placebo patients and their stented counterparts. This brings into question both the validity of stenting for this indication and the tens of millions of dollars that have been spent on this treatment over the years.
The results of this trial may prove to be cause for concern for patients and healthcare providers everywhere. It is impossible to estimate how many patients have received sub-par procedures, and how much money has been wasted on inferior treatments. GlobalData believes that the results of this study will emphasize the medical community’s need to be more rigorous in the future when evaluating the respective strengths of its treatments.