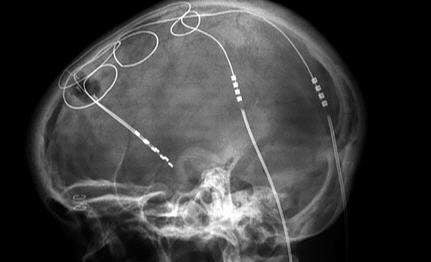
When an obese patient with type two diabetes underwent treatment for obsessive-compulsive disorder (OCD) using deep brain stimulation (DBS), a surprising side effect was discovered. The patient’s diabetes significantly improved, with a drastic reduction in his daily insulin intake. This unexpected outcome was investigated further in a recent study in Amsterdam, published by Science Translational Medicine in order to determine whether DBS was the direct cause of the improvement.
DBS is a neurosurgical procedure wherein a neurostimulator, also referred to as a “brain pacemaker”, is implanted in the patient’s body. This implanted device is then programmed to deliver electrical pulses to specific targets of the brain. The procedure can be used to treat OCD as well as other neurological disorders. Using DBS for OCD treatment results in an increase in the levels of dopamine, a neurotransmitter that helps to control the brain’s reward and pleasure centers. Researchers believe that this boost in dopamine impacts the body’s ability to metabolize sugar.
In the study, 14 people who had already undergone DBS treatment for OCD but did not suffer from type two diabetes were recruited. The DBS devices were turned off for 17 hours and blood sugar levels were monitored. The researchers discovered that DBS therapy increased insulin sensitivity, as turning off the brain stimulators corresponded to higher insulin levels. In a separate rodent experiment, the researchers stimulated dopamine-releasing neurons in mice; similar results were attained, as increased dopamine production led to a higher glucose tolerance.
A relationship between the central dopamine system and insulin sensitivity in humans has been proposed before, but it has been difficult to establish the underlying mechanisms. Whether these recent findings will lead to the utilization of DBS as a definite treatment for diabetes therefore remains to be seen.