According to the World Health Organization (WHO), breast cancer (BC) is both one of the most common cancers in the world and the most common cancer in women worldwide, accounting for approximately 25% of all incident cases of female cancers.
Preventative measures intended to improve BC survival, such as organized nationwide mammography screening, have recently been implemented. These measures are expected to improve survival, as well as impact the incidence and prevalence of the disease. Additionally, advances in genomic medicine have led to preventive treatment by testing high-risk individuals for the genetic markers BRCA1 and BRCA2.
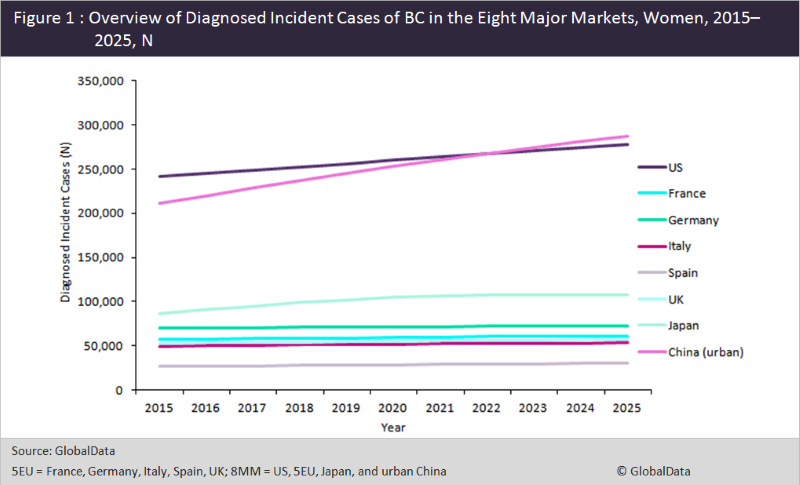
According to GlobalData’s epidemiological forecast, the diagnosed prevalent cases of invasive BC are expected to increase from approximately 795,000 cases in 2015 to 949,000 cases in 2025 in the eight major markets (8MM = US, France, Germany, Italy, Spain, UK, Japan, and urban China) (Figure 1). In light of this expected increase in incident cases of BC, preventative measures such as mammography screening and genetic testing will become increasingly important in reducing the burden of the disease. In fact, an article published in The Journal of the National Cancer Institute in January assessed the cost-effectiveness of genetic screening for the entire population and found that population-based screening for several breast and ovarian cancer genetic mutations was more cost-effective than screening the high-risk population for BRCA1 and BRCA2 genetic mutations alone.
The study, which was led by the London School of Hygiene & Tropical Medicine, Barts Cancer Institute at Queen Mary University of London, and the Barts Health NHS Trust, demonstrated that implementing a population-wide screening program in women over 30 years of age had the potential of reducing approximately 1.86% and 1.91% of BC and 3.2% and 4.88% of ovarian cancer in the UK and the US, respectively. These findings could mean a change in the guidelines for BC genetic testing from only screening high-risk individuals to screening the whole female population. Details about the trend analysis and other discussions of BC epidemiology can be found in GlobalData’s EpiCast Report: Breast Cancer – Epidemiology Forecast to 2025, and in GlobalData’s EpiCast Model: Breast Cancer – Epidemiology Forecast to 2025.

Related Reports
- GlobalData (2016). EpiCast Report: Breast Cancer (HER2+, HER2-) – Epidemiology Forecast to 2025, December 2016, GDHCER133-16
- GlobalData (2016). EpiCast Report: Ovarian and Primary Peritoneal Cancer – Epidemiology Forecast to 2025, December 2016, GDHCER138-16
For more insight and data, visit the GlobalData Report Store – Medical Device Network is part of GlobalData Plc.