Since the 1980s, an increasing number of medical device products have been labelled ‘single-use’, designed to be used once, on one patient, and to then be discarded. The result was that products could be made more cheaply, and being used just once meant ensuring product sterilisation was no longer an issue. However, the practice has since become so widespread that some are asking whether single-use medical device manufacturing has become akin to planned obsolescence.
Planned – or built-in – obsolescence is the practice of designing a product with an artificially limited lifespan, so that it becomes obsolete after a certain amount of uses or a specific amount of time. The European Union (EU) has recently been cracking down on planned obsolescence in the consumer world, with Apple investigated in France over intentionally shortened iPhone lifespans.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
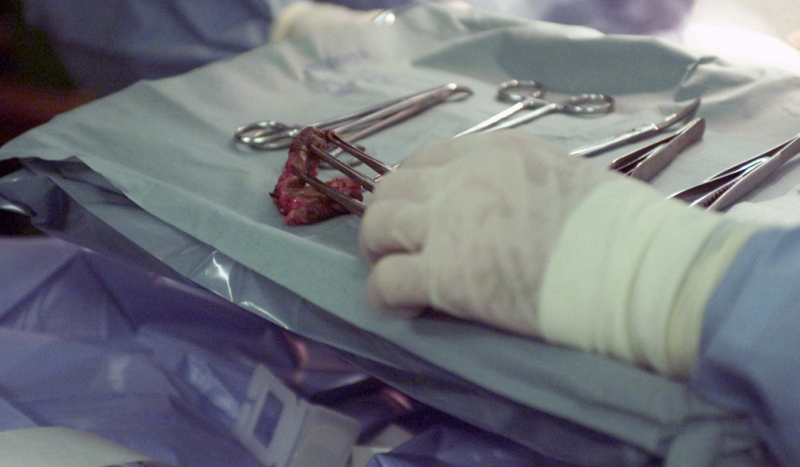
Single-use device (SUD) reprocessing for medical devices has become a widespread practice for non-invasive and minimally invasive devices, such as compression sleeves, tourniquet cuffs, scissors, forceps, scalpels and cardiac catheters, with dedicated companies cleaning, disinfecting and repurposing used SUDs. The process saves hospitals a significant amount of money, and is US Food and Drug Administration (FDA) approved when carried out correctly to specific guidelines. But, a growing amount of medical devices are now being designed with integrated technology, such as electronic chips, that inhibit reuse and reprocessing, eliminating any hospital cost-saving.
Reprocessing: a new lease of life
When SUD reprocessing was first established in the 1980s, hospitals were carrying out the process themselves as a cost-saving measure. But by the early 2000s the FDA decided that though reprocessing was not unsafe, regulation was still required to ensure patient safety.
“Some devices cannot be used more than once due to material degradation, technical limitations and patient safety. This is why we have the ‘single-use’ designation, and it is validly used to ensure patient safety and patient care efficacy,” explains device reprocessing firm Innovative Health’s vice-president of marketing and public affairs Lars Thording. “However, a small amount of single-use devices can be re-used, after going through stringent and controlled procedures. It is very possible that original manufacturers in some cases apply the single-use label to increase sales and ensure obsolescence.”
FDA oversight means SUD reprocessing is subject to the same level of regulation that original equipment manufacturers adhere to; if anything, reprocessors face even more stringent oversight to ensure re-used devices are equivalent to their original counterparts. “Thanks to tight regulations, patient safety is not an issue,” says Thording. “It has, in fact, been demonstrated that new devices fail more frequently than reprocessed ones.”
In reality, only a very small number of SUD devices are suitable for reprocessing. According to Thording it is an enormous engineering and regulatory challenge to receive FDA clearance, but while he comments that this is a good thing for patient safety, he says there is untapped potential in the medical device market.
“There is still large potential for more single-used devices to be reprocessed, which can significantly add to the savings already achieved by hospitals,” he says. “However, for more single-use devices to be reprocessed there must be greater insistence on the part of the hospital that device costs need to come down and willingness in the reprocessing industry to make the investments.”
Chipping devices to halt reprocessing
Reprocessing itself is a costly process, as a substantial amount of research and development needs to go into repurposing devices, but compared to investing in new technology, hospitals can save a significant amount of money by using reprocessed SUDs.
Thording explains that “the investment in R&D and regulatory affairs associated with getting FDA clearance is substantial, and engineering teams often must work for three to four months to submit FDA clearance.
“Yet it is still a lot less expensive than manufacturing the original device, which is why hospitals can realise substantial savings – some facilities more than $1m per year. Reprocessing is not a low-cost activity; however hospitals can still generate significant savings, as reprocessed devices cost 40%-60% less than a new device.”
But, because SUD reprocessing cuts into the profits of the associated original equipment manufacturers, some are implementing techniques to block advancements in the field.
“[As an example,] sensor-enabled catheters in the cardiology space are extremely expensive, and manufacturers invest heavily in chipping and locking the devices so they can’t be reprocessed,” says Thording. “Thankfully some of the more advanced reprocessing companies are able to ‘break the locks’ and secure the hospital savings. Some of these catheters cost $2,000-$3,000 or more.”
There is no clinical rationale for such ‘locks’, and the result is simply more expensive devices that cost hospitals more money. And the problem isn’t set to dissipate – when new devices are developed, they are priced even higher than current technology, which will gradually be phased out, resulting in steadily rising prices and a monopolised market.
But how can the problem be solved? According to Thording, rather than policymakers or manufacturers, the power lies with the hospitals themselves. “Hospitals are really in a position to make the biggest difference. When manufacturers push expensive devices to the hospitals, they have the ability to stand up and say ‘no’.
“By refusing to purchase new products with few technical or clinical advancements and which are designed to prohibit reprocessing, hospitals can support this practice, thus reducing costs significantly.”





