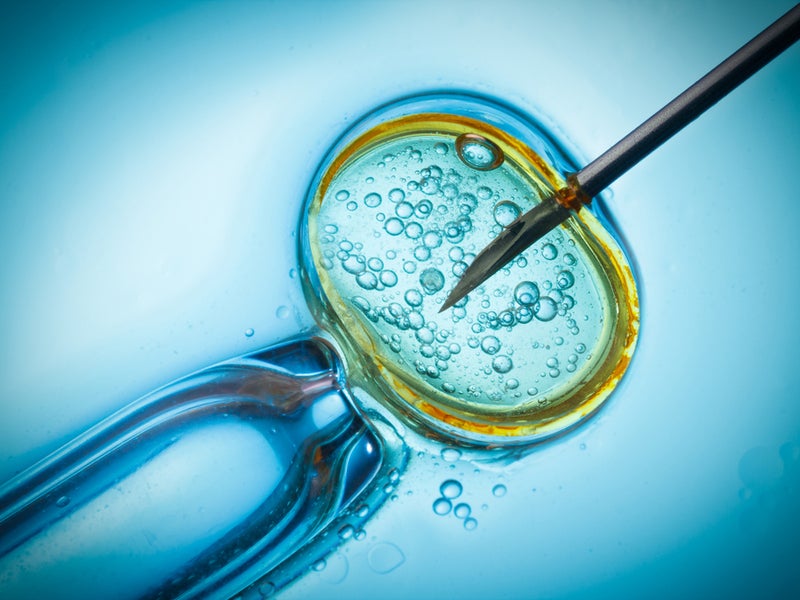
Since the first baby conceived through in vitro fertilisation (IVF) was born in 1978, more than 8 million people globally have been born using the technology. While IVF success rates have improved since it was first introduced, currently, only about a third of patients have a successful live birth.
“For patients, assisted reproduction is prohibitively expensive, often requires multiple attempts, is physically and emotionally onerous, and is still rarely covered by insurance,” relays Paxton Maeder-York, CEO and Founder of Alife Health.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Equitable access and affordability in the fertility treatment space are leading barriers to IVF. In the US, it has been reported that only one in twenty-five couples has access to the fertility care they need. An average IVF cycle costs between $15,000 to $30,000, limiting the number of people who can access quality care.
“People want fertility treatments to be accessible, affordable, effective and less stressful,” says Meir Olcha, fertility specialist, Mira medical advisor and medical director at Sama Fertility. “This is where technology can be a gamechanger in our field.”
Consumers, clinicians and care
Within the clinical environment, it is recognised that historically, research and development (R&D) in women’s health and infertility have been underfunded. Recent advances have therefore mostly come from private-sector fertility clinics. However, the space has recently attracted more attention from investors and technology innovators, many of whom were motivated by their personal experiences.
“Despite the astonishing advances in assisted reproduction in the last few decades, outcomes are still frustratingly suboptimal,” says Gary Nakhuda, co-founder of Olive Fertility Center in Canada. Ongoing demand for the latest innovations that provide even the slightest marginal improvement in success rates therefore persists.
Beyond the outcome, the primary expectation is to improve the overall patient experience during fertility treatment. Clinics face significant obstacles in delivering the best possible fertility care. Successful pregnancies from IVF rely on a complex set of clinical decisions made by physicians to provide optimal care for each patient.
“Evidence shows that major stressors for patients are the requirements for frequent clinic visits, invasive tests and communication issues with clinic staff during treatment,” says Nakhuda. Focusing on the operational aspects of delivering care is crucial to reducing patient drop-out and maintaining engagement with care, which Nakhuda says “is very often the key to persisting until a successful outcome is reached.”
Fertility tools advancing the field
New technologies to optimise clinical care and improve clinic operations can help propel the field forward to support more patients in achieving successful outcomes. “Today, there is no unified technology platform working to help doctors optimise those decisions and improve the patient experience,” says Maeder-York.
From a technology perspective, the latest advancements in fertility health focus on bringing clinical data and workflows to the digital era. Electronic witnessing systems that use barcodes to ensure the proper tracking of sperm, eggs and embryos, robotic cryopreservation systems and artificial intelligence-led (AI) tools are helping to progress reproductive health.
Today’s sophisticated tools build upon the past decade’s advancements in three major categories: embryology laboratory, at-home testing and monitoring and AI. The post-pandemic landscape expands opportunities as people embrace telehealth, virtual care and the trend toward at-home testing accelerates.
“All advancements are aiming for the same thing – to improve quality of care and clinic efficiencies through data and software technology,” says Maeder-York.
Navigating limitations of current technology
IVF is an important and relatively new area of medicine that is still developing quickly. “Advanced analytics and improvements enabled by AI will have an important impact on the continued evolution of what the process looks like for patients,” says Maeder-York. By aggregating and interpreting data, AI may help to improve fertility treatment outcomes, reduce costs and make the entire IVF process more transparent.
“Age and limitations of human biology are simply the most difficult challenges,” says Nakhuda. Yet, even with a simple hormone test such as an Anti-Müllerian hormone (AMH), early testing can help make some reproductive decisions. The hope is that emerging knowledge will help personalise treatment even further.
Sophisticated reproductive health technologies offer opportunities to push fertility health forward. Moving to a patient-centric approach coupled with insightful clinic-to-patient collaboration can lead to a more supported, holistic and positive IVF experience.
Alife Health has found that, on average, clinics spend a combined three weeks per quarter having their staff data mine and build reports. While there is a tremendous amount of data available, problems in sorting, extracting and digesting to transform into actionable insights prevail. Technologies that collect, digitise, organise and provide key information in real-time are entering clinics to bring essential fertility information and trends to the fore.
In a study conducted by the brand, researchers stated that using a machine learning model for selecting starting follicle-stimulating hormone (FSH) can achieve optimal laboratory outcomes while lowering the amount of starting and total FSH used.
In addition, embryologists typically have a manual process for reporting on embryo quality. They will grade embryos while looking through a microscope, transcribe information into their electronic medical record (EMR) systems and generate reports. Embryo image capture systems can simplify image capture, storage and organisation of embryo images while improving the efficiency of the grading process by syncing with EMR.
Progressing fertility health
Digital-first care delivery is becoming a priority. However, unlike pure digital health platforms for functions such as medication prescribing, fertility care has to be tied to a brick-and-mortar facility where treatments can physically occur, says Nakhuda. Innovative platforms allow for remote testing, monitoring and decentralising much of the process of patients’ experience of treatment burden relief.
During IVF, healthcare professionals, including doctors, laboratory technicians and embryologists, are tasked with making many decisions to improve a patient’s chance of success. “IVF isn’t a single medical procedure to help with infertility but, rather, a complex series of procedures,” says Maeder-York.
When designing its AI-led fertility tools, Alife Health wanted to help doctors and fertility specialists optimise patients’ IVF process, deliver optimal results throughout treatment and reduce the overall cost of care so more people can access it as the need continues to grow.
In March 2022, Alife Health received a $22 million investment. With its aim to create a complete operating system for the next generation of IVF care delivery, the AI-led brand has transitioned from its R&D phase into early traction and commercialisation. In October 2022, the company launched its AI platform to support and enhance clinical decision-making for IVF patients throughout the process, including during ovarian stimulation and embryo grading. In 2023, Alife Health plans to release two patient products that focus on providing health equity in the IVF space by helping people regardless of where they seek treatment.
Pursuing the at-home remote monitoring trend, Mira device allows for quantitative measurement of hormones in the urine, as opposed to the traditional approach of blood sampling, which is both inconvenient and painful. Collaboration between fertility tech and clinics is also one way to improve patients’ reproductive health outcomes and the landscape. The fertility tech brand has teamed up with fertility clinics in the US, Canada and Australia to make fertility care more accessible by reducing the number of patient visits and minimising testing costs.
Canadian fertility clinic, Olive Fertility Center, has recently completed a trial with IVF patients in collaboration with Mira. The trial showed that urinary oestrogen dynamics measured with the device were comparable to those measured with serum oestrogen, demonstrating that at-home urine monitoring can be a valuable alternative to blood tests for patients undergoing IVF.
Future of fertility treatment
While “it is early days”, Nakhuda says advanced technology like AI seems to have many use cases in fertility, from selecting the best treatment options to dosing medication protocols, interpreting imaging results and predicting the quality of gametes and embryos.
We can expect to see more patients utilising these advancing technologies and advocate for broader adoption as healthcare widely recognises its value.
“There is no reason to believe that we won’t surpass or at least optimise human decisions, which are always subject to bias and noise,” says Nakhuda. Automated laboratory techniques are, therefore, on the horizon. Implementing these innovations will optimise outcomes and scale access to care, therefore overcoming the paucity of trained providers and scientists required for these complicated tasks.
The prospect of at-home ultrasonography that can be self-administered by the patient and interpreted remotely by the physician is now a possibility. “It is a huge step forward in making hormone tracking during fertility treatments more patient-friendly, convenient and less intrusive,” says Nakhuda.
Soon, patients won’t have to wait months to get a diagnosis, leave their house and travel extensively to get excellent medical care. “This is the era where patients get diagnosed faster and treated better as we see access improve,” says Olcha.
Personalised fertility treatment is the next area to breakthrough. Describing it as the “quantum leap” continuing in genomics, Nakhuda states it will also influence fertility care, allowing truly personalised medicine, screening of reproductive risk factors and improved selection of healthy embryos.
Growing awareness of infertility and consciousness for fertility preservation strategies such as oocyte and embryo vitrification are also at the forefront of developments. Reproductive health professionals hope it may also help mitigate formidable biological limitations of age which, Nakhuda shares, “we are still far from being able to overcome”.
As new technologies develop, whether in the laboratory or with a patient, we must ensure that tests are validated and effective. “We have to ensure that at-home testing technologies are at least as accurate if not more accurate than the gold standard tests currently used,” says Olcha.





