Materials Used in the Medical Implant Industry
Materials used in medical implants vary from the well-known to the obscure. The following is a collection of some of the most common and innovative medical implant materials, ranging from familiar silicone to new 3D-printed bio-materials.
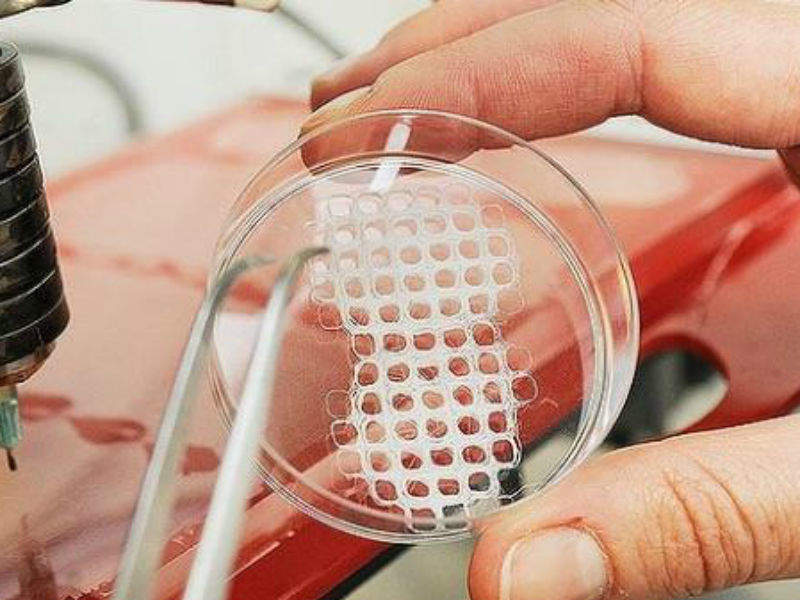
Surgical mesh


Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Surgical mesh is made from both inorganic and biological materials which are loosely woven together to form a sheet. These sheets can be used as either temporary or permanent support for organs or various other tissues during surgery. It is most commonly used for hernia or gynaecological repair. Permanent versions of the mesh can stay in the body forever whereas temporary ones often dissolve away.
The material has been in the news recently as, like with many materials used in medical implants, the safety of its use and potential side effects have come into question. A rheumatologist from the University of Alberta in Canada found that high reports of autoimmune disorder symptoms in patients could be due to surgical mesh implants.
Silicone
![]()
Silicone gel is an inert polymer which causes no known human allergies or reactions. The material is usually heat-resistant and can be liquid or rubber-like in texture. It is well-known for being used to make breast implants for reconstructive surgeries and is often chosen over saline breast implant options despite the higher risks should leakage of silicone into the body occur. The first silicone breast prosthesis was created in the 60s. As with surgical mesh, silicone has come under scrutiny for complications such as breast implant-associated anaplastic large-cell lymphoma.
Silicone is also used to make other medical implants such as tracheal stents and, according to recent reports, the silicone tracheal stent market is set to grow.
Polyethylene

Almost all total knee replacement implants and many total hip replacement implants contain ultra-high molecular-weight polyethylene (UHMWPE). This plastic is necessary to provide cushioning and movement. Polyethylene is the most common plastic and it is often one of the materials used in medical implants because it is a porous synthetic polymer that is biologically inert and does not degrade in the body.
However, some polyethylene implants are considered better than others. A long-term follow-up study conducted in Australia confirmed that hip implants which contain crossed-linked polyethylene (XLPE) substantially lower the risk of a patient requiring revision surgery after a total hip replacement when compared to the effects of implants that contain the conventional polyethylene (CPE) components.
High density polyethylene (HDPE) solid implants have been used by plastic surgeons since the 80s for facial augmentation purposes.
Titanium

Titanium is often used to make implants for dental surgery but has more recently been used instead of stainless steel for other medical uses, such as hip implants. Titanium is a non-allergenic and biocompatible material. It is also used to make heart valves and bone screws. Its main advantage when used to fix bones is that it can integrate with bone and is extremely strong but lighter than most alloys.
Despite being erosion-resistant and incredibly strong, titanium plates can lead to bone embrittlement once bones are healed as the material is significantly more rigid than bone. Early this year scientists in Japan developed titanium fibre plates that are safer than conventional titanium plates when used to support broken bones.
Polyurethane foam

In the field of materials used in medical implants, polyurethane foam is a fairly new addition. Researchers from the Hong Kong Polytechnic University created a scaffolding implant that encourages the regeneration of bone by combining shape memory polyurethane foam along with the bone tissue component hydroxyapatite.
Polyurethanes have a number of medical applications including catheter tubing, wound dressings and injection moulded devices but their most common use is in short-term implants. The material has been used as a coating for some breast implants, although there have been calls for a safer, non-biodegradable material to be found as an alternative.
Image Credit: The Hong Kong Polytechnic University.
Polylactic acid

As mentioned above, if a screw is used in a surgical operation it will likely be made of titanium. However, patients with titanium screws often have to have a second operation to have them removed. To avoid this, surgeons have started to use polyactic screws because they are biocompatible and biodegradable. One of the few issues with these screws is that sometimes the biodegrading process can leave holes in the bones they were intended to fix. Researchers at the Fraunhofer Institute for Manufacturing Engineering and Applied Materials Research (IFAM) in Bremen offered a solution to this by combining hydroxylapatite with polylactic acid to create a mouldable composite which can be used to make medical screws that also promotes bone growth into the implant.
Image Credit: Fraunhofer IFAM.
3D-printed bio-materials

This category of materials used in medical implants is the broadest as scientists continue to discover implantable materials that can be 3D-printed for medical purposes. 3D cell printing with a microfluidic approach has resulted in significant leaps in the vascularisation of engineering tissues. With the use of biomaterials and polymerisation techniques, precise replications of human tissues can now be replicated.
A 3D printing Biopen device called Biosphere has recently been developed by researchers in Australia. The technology is essentially a device filled with stem cell ‘ink’ that allows surgeons to repair damaged bone and cartilage by drawing new cells directly into any damaged areas of bone during surgery.
Image Credit: Open Biomedical Initaitive.





