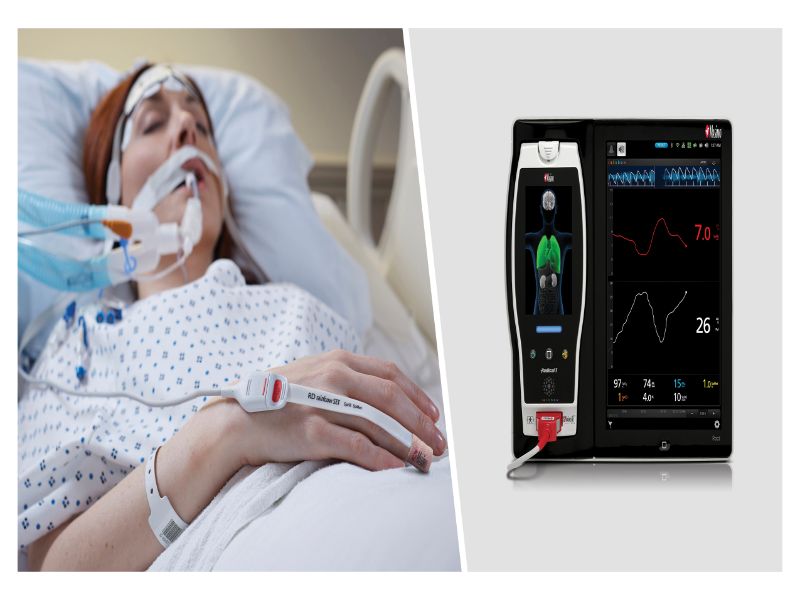
The US Food and Drug Administration (FDA) has approved Masimo’s Pleth variability index (PVi) as a continuous, noninvasive, dynamic indicator of fluid responsiveness in select populations of mechanically ventilated adult patients.
PVi is a measure of the dynamic changes in perfusion index that takes place during the respiratory cycle.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Masimo’s proprietary algorithm developed based on the relative variability of the pleth waveform is used to calculate PVi.
It is offered alongside Masimo SET pulse oximetry and rainbow Pulse CO-Oximetry on a variety of 2-LED, 4-LED and 8-LED Masimo sensors.
Masimo founder and CEO Joe Kiani said: “We are thrilled that at long last we are able to offer clinicians and patients in the US the full benefits of PVi monitoring.
“Multiple studies have shown how this breakthrough noninvasive indicator of fluid responsiveness can help improve outcomes and reduce costs on mechanically ventilated patients with no more equipment needed than a software upgrade with most existing Masimo SET and rainbow platforms and the existing Masimo SET sensors that so many top hospitals around the world already use for pulse oximetry.”
Fluid management is recommended by hospital protocols such as enhanced recovery after surgery (ERAS) and goal-directed therapy (GDT) as part of larger initiatives for the enhancement of patient care and safety.
Furthermore, fluid management protocols are designed to balance fluids by recognising when patients may be fluid-responsive.
The accuracy of PVi in forecasting fluid responsiveness is said to be variable and influenced by various patient, procedure and device-related factors. While it measures the variation in the plethysmography amplitude, it does not offer measurements of stroke volume or cardiac output.
PVi has been used in combination with Masimo’s noninvasive, continuous haemoglobin monitoring technology (SpHb), the company said.
A study found that use of an integrated GDT algorithm, using both PVi and SpHb, resulted in earlier transfusion and fewer units of blood transfused. It also noted a 33% lower mortality rate 30 days after surgery and a 29% lower mortality rate 90 days after surgery.





