Need to Know:
- Wearables can be a value-added aspect to data collection in clinical trials, to complement electronic Patient Reported Outcomes and electronic Clinical Outcome Assessments.
- Central nervous system and cardiovascular spaces continue to be on top in integrating wearable or sensor devices in clinical trials, but rare diseases and oncology are not far behind.
- FDA guidance on validation for wearables exists but the onus is on makers and sponsors to seek additional regulatory guidance.
The boon of remote monitoring such as sensors and trackers in decentralised clinical trials (DCTs) shows no sign of slow down, but the onus is on wearable makers as well as study sponsors to ensure there is proper device validation.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
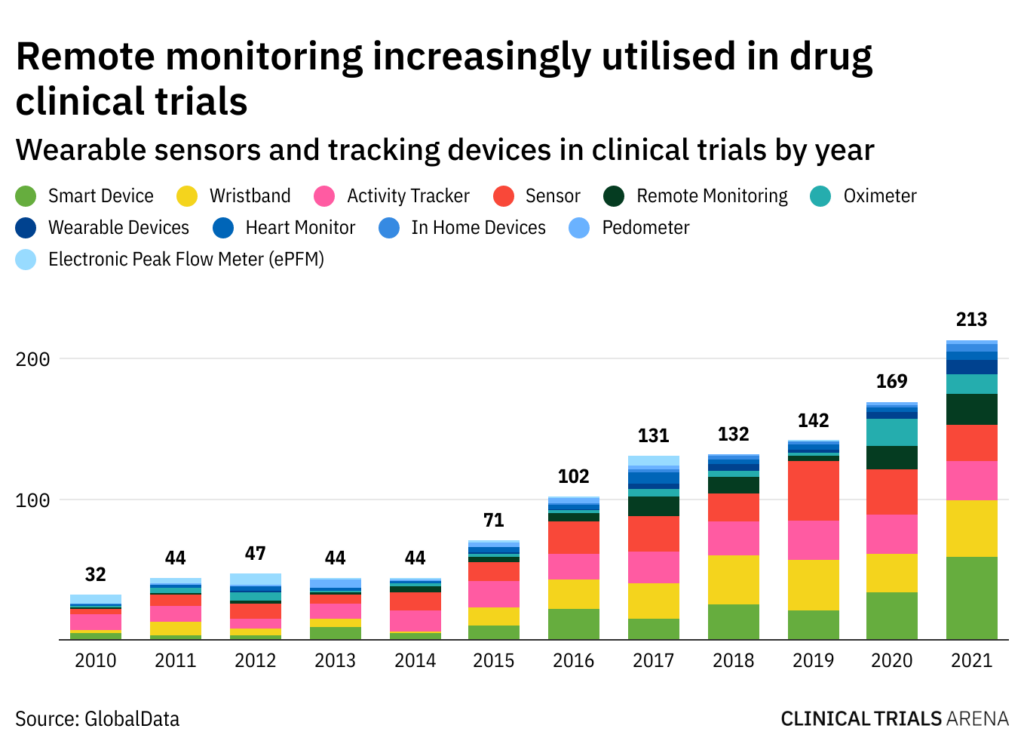
As reported in an exclusive analysis by Clinical Trials Arena, wearable sensors and tracking devices in DCTs averaged at 42 clinical trials per year between 2010 and 2014. But this has consistently increased starting in 2015, breaking the 200-study mark last year. The biggest jump was seen between 2020 and 2021, rising by 44 trials from the previous year. Remote monitoring that involves wearables are designed to track trial participant outcomes between regular onsite visits, while also reducing overall visit numbers.
In an advance in the DCT landscape, long-established assessment tools such as electronic Clinical Outcome Assessment (eCOAs) are now supported by wearable sensors and tracking devices. Wearables enable a broader view of the patient journey as it complements and enhances electronic Patient Reported Outcome (ePRO) collections, adds Nico O’Kuinghttons, vice president of commercial, DCTs at Huma.
The different digital solutions can allow for broader and better data collection, O’Kuinghttons says. Algorithms allow for information collection that can complement and allow a fuller assessment of surrogate endpoints.
To keep reading this analysis, and view the interactive graph above, visit Clinical Trials Arena by clicking this link. Clinical Trials Arena is a sister publication of Medical Device Network